Abstract
Background. Maxillary expansion is one of the treatment options for the correction of the skeletal constriction of the upper jaw. However, evidence regarding the best treatment effects with the use of rapid vs. slow maxillary expansion in the early adolescence period (i.e., between the age of 12 and 16 years) is still lacking in the available literature.
Objectives. The aim of the present study was to investigate the effectiveness of rapid and slow maxillary expansion in treating posterior skeletal constriction, and to compare the 2 techniques in terms of skeletal and dentoalveolar changes by using cone-beam computed tomography (CBCT).
Material and methods. The sample consisted of 34 patients (15 males and 19 females) suffering from posterior skeletal constriction. They were randomly allocated either to the rapid maxillary expansion (RME) group (17 patients aged 13.76 ±0.32 years) or to the slow maxillary expansion (SME) group (17 patients aged 14.02 ±0.28 years). The skeletal and dental landmarks, and changes in the posterior dimensions were examined using CBCT radiographs at the beginning of treatment (T1) and at the end of the observation period (T2).
Results. There were no significant differences between the 2 groups in terms of skeletal and dental changes except the amount of change in the inter-premolar width at the root apex, which was greater in the SME group (p = 0.007), as well as the amount of change in the skeletal palatal width in the molar region, which was also greater in the SME group (p = 0.008).
Conclusions. Both maxillary expansion protocols were effective in treating posterior skeletal constriction. The average changes in the skeletal and dental widths were generally similar in both groups. Therefore, SME can be considered as an alternative to RME in patients with skeletal maxillary constriction in the early adolescence period.
Keywords: cone-beam computed tomography, maxilla, palatal expansion technique, constriction
Introduction
Maxillary constriction is a common orthodontic problem, which can be found at any age.1 It appears clinically as maxillary constriction accompanied by the presence or absence of dental crowding.1, 2 Maxillary expansion is the first treatment option for this skeletal defect of the upper jaw.1 There are many types of maxillary expansion, depending on the applied force and the number of expansion times: rapid maxillary expansion (RME); semi-rapid maxillary expansion (SRME); and slow maxillary expansion (SME).1 Maxillary expansion consists in increasing the width of the jaw by opening the palatal suture.1, 2 In cases where palatal suture fusion is encountered, surgically-assisted rapid maxillary expansion (SARME) can be used, and this method is considered an appropriate alternative solution for adult patients.3, 4
Rapid maxillary expansion is based on a major and intermittent force system that leads to the dentoalveolar tipping of the posterior teeth.5 It has recently taken priority as a treatment option for the skeletal posterior cross-bite.2 Nevertheless, numerous side effects have been reported for this procedure, such as pain, relapse, molar inclination, bone loss, gingival recession, and root absorption.6 On the contrary, SME is associated with less resistance of the skeletal structures and better bone formation within the median palatal suture, thereby mitigating the side effects of RME.6
Both RME and SME are considered treatment options available to growing patients between the age of 9 and 12 years.2 Some researchers have supported the use of RME in the early mixed-dentition period.7, 8 Several studies have been conducted to compare RME and SME in the late mixed-dentition period, and most of them have found that both types of expansion bring similar results.2, 9 On the other hand, the choice of the expansion protocol in older age is more difficult, taking into account midpalatal suture ossification.2 The availability of modern computerized tomography systems, which provide high accuracy with minimum radiation exposure, has enabled a thorough analysis of the maxillofacial complex components, as well as precise linear and angular measurements.2, 10 Several studies have compared RME and SME in early childhood, i.e., between the age of 6 and 9 years.9, 11 Other studies have compared the 2 types of expansion in the late mixed-dentition period, i.e., at the age of 9–12 years.5, 12 After the radiological assessment of patients aged 9–12 years, Martina et al. found that RME was similar to SME with regard to skeletal and dental measurements.5 Their results indicated the advantage of SME over RME, as the complications of RME could be avoided.5 However, no previously published research has attempted to study the feasibility and effectiveness of RME in comparison with SME in the early adolescence period, i.e., the early permanent-dentition period.
Therefore, this trial aimed to compare the transverse skeletal and dental changes following RME and SME in early adolescent patients (i.e., between the age of 12 and 16 years) by using cone-beam computed tomography (CBCT) imaging.
Material and methods
Study design and registration
This study was a single-center randomized controlled trial with a two-arm parallel-group design, comparing RME and SME in early adolescent patients. Patients attending the Department of Orthodontics at the Dental School of the University of Damascus, Syria, between July 2017 and June 2018 were screened for inclusion. The study was approved by the institutional Research Ethics Committee at the University of Damascus (UDDS-2675-15,032,017/SRC-4771). The trial was retrospectively registered at ClinicalTrials.gov (ID: NCT03667508).
Sample size calculation
The sample size was determined using Minitab®, v. 17 (Minitab, State College, USA), assuming a 2-millimeter difference in the maxillary basal width between the 2 groups (RME and SME) as clinically significant. The variability of this measurement was about 2.2 mm in a previously published study.5 Using the independent-samples t tests with a significance level of 5% and a power of 80%, 16 patients were required in each group. One patient was added to each group to avoid any potential attrition, bringing the total number in each group to 17 patients.
Patients’ recruitment and eligibility criteria
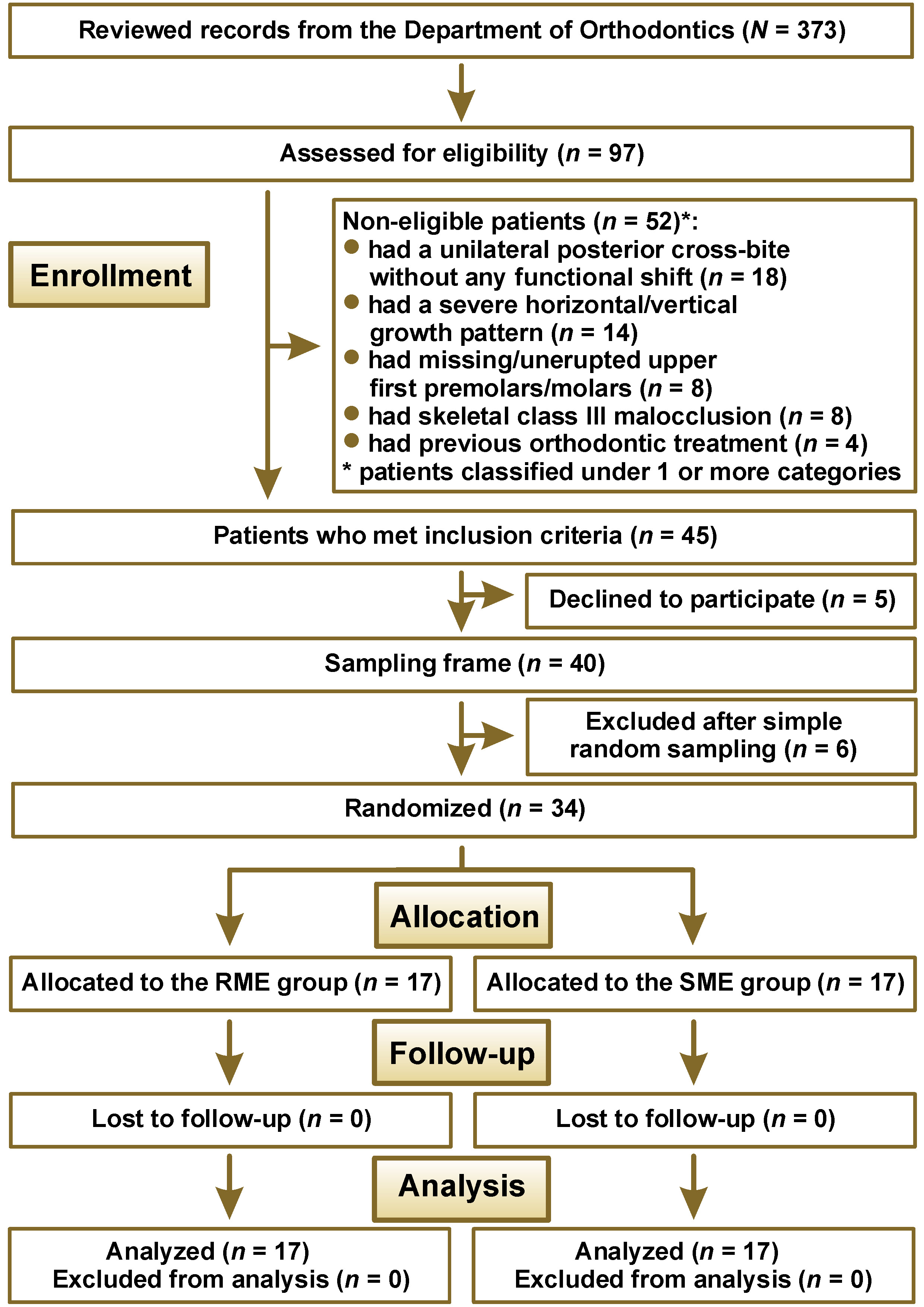
After examining 97 patients attending the Department of Orthodontics, 45 patients met the inclusion criteria and the research project was explained to them. From among the 40 patients who agreed to participate in the study, 34 (15 males and 19 females) were randomly selected (Figure 1).
Information sheets were given to all patients and informed consent forms were collected upon approval. The inclusion criteria were as follows: patients in the early permanent-dentition period; chronological age between 12 and 16 years; presence of a functional unilateral posterior cross-bite (with a functional shift) or a bilateral posterior cross-bite (without any functional shift); bilateral upper jaw constriction (symmetric constriction) assessed clinically, and then confirmed radiographically; dental and skeletal class I and II malocclusion; normal and mild vertical growth pattern; no general health problems; and good oral health. The exclusion criteria were as follows: presence of periodontal diseases; presence of general diseases, syndromes or cleft lip and palate; presence of a unilateral posterior cross-bite without any functional shift; severe horizontal/vertical growth pattern; missing/unerupted upper first premolars/molars; skeletal class III malocclusion; and previous orthodontic treatment.
Randomization, allocation concealment and blinding
The patients were distributed between the 2 groups using a list of random numbers generated by the Minitab software, with an allocation ratio of 1:1. The 34 patients were distributed randomly into 2 groups: the RME group (n = 17); and the SME group (n = 17). The allocation sequence was hidden by using opaque sealed envelopes. The blinding of patients and practitioners was not viable. Thus, blinding was used only for data analysis. The 1st group received RME, whereas the 2nd group received SME (Figure 1). One of the academic staff members, not contributory to this study, was responsible for the generation of the random allocation sequence and the insertion of the participants into the 2 groups.
RME group and the activation protocol
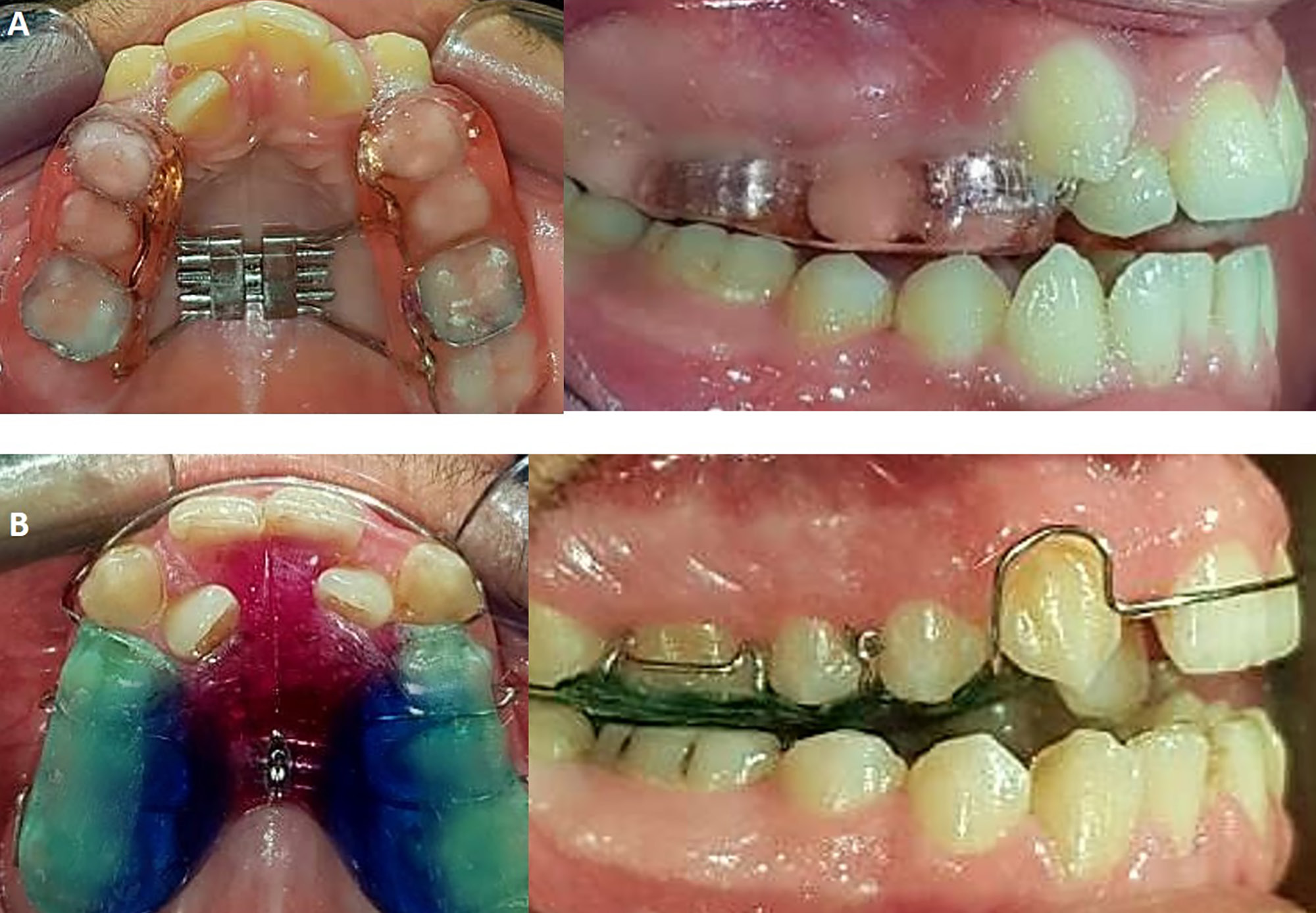
The RME expander used in the current study was a modified Hyrax bonded rapid palatal expander with occlusal splints. Bonding was accomplished by using a conventional glass-ionomer cement (GIC) (Ketac™ Cem; 3M ESPE, Seefeld, Germany) on first premolars and first molars (Figure 2A). The patient activated the expander twice daily (these 2 movements produced half of a full screw turn, equivalent to 0.4 mm),13 until an overcorrection of maxillary constriction of approx. 2–3 mm was obtained.14 The expander was left in its place for 3 months as a retention period,15 and then, after removing the appliance, a CBCT image was taken.
SME group and the activation protocol
The SME expander used in the current study was a removable palatal expansion appliance consisting of posterior bite planes and a midline split incorporating 1 expansion screw (Figure 2B). The patient activated the expander twice weekly,13 until an overcorrection of maxillary constriction of approx. 2–3 mm was achieved.14 The expander was left in its place for 1 month as a retention period,5 and then, after removing the appliance, a CBCT image was taken.
There was no change in either group regarding the treatment procedures. The planned treatment protocol prior to the start of the trial was strictly followed until the end of the treatment follow-up.
CBCT image acquisition and analysis
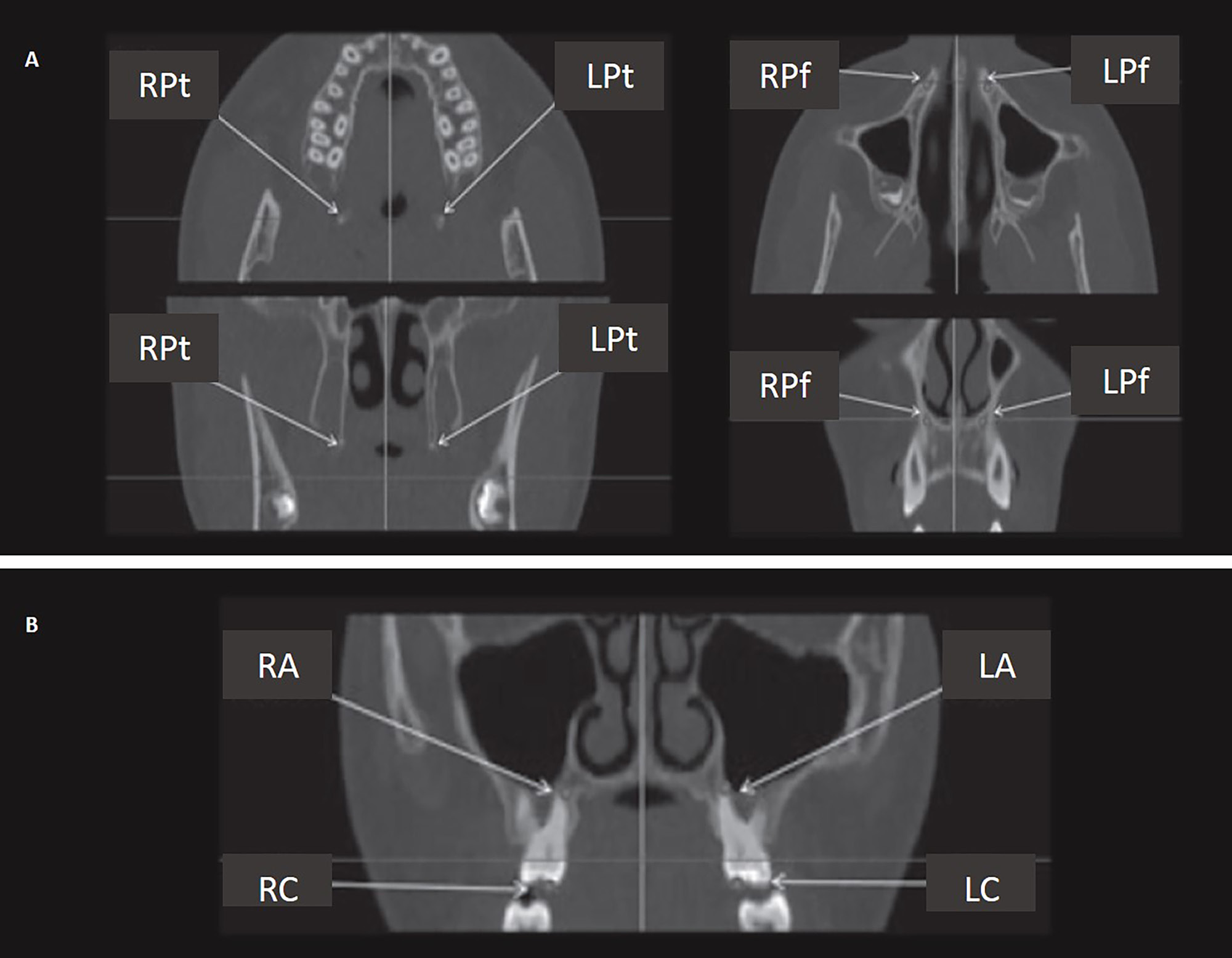
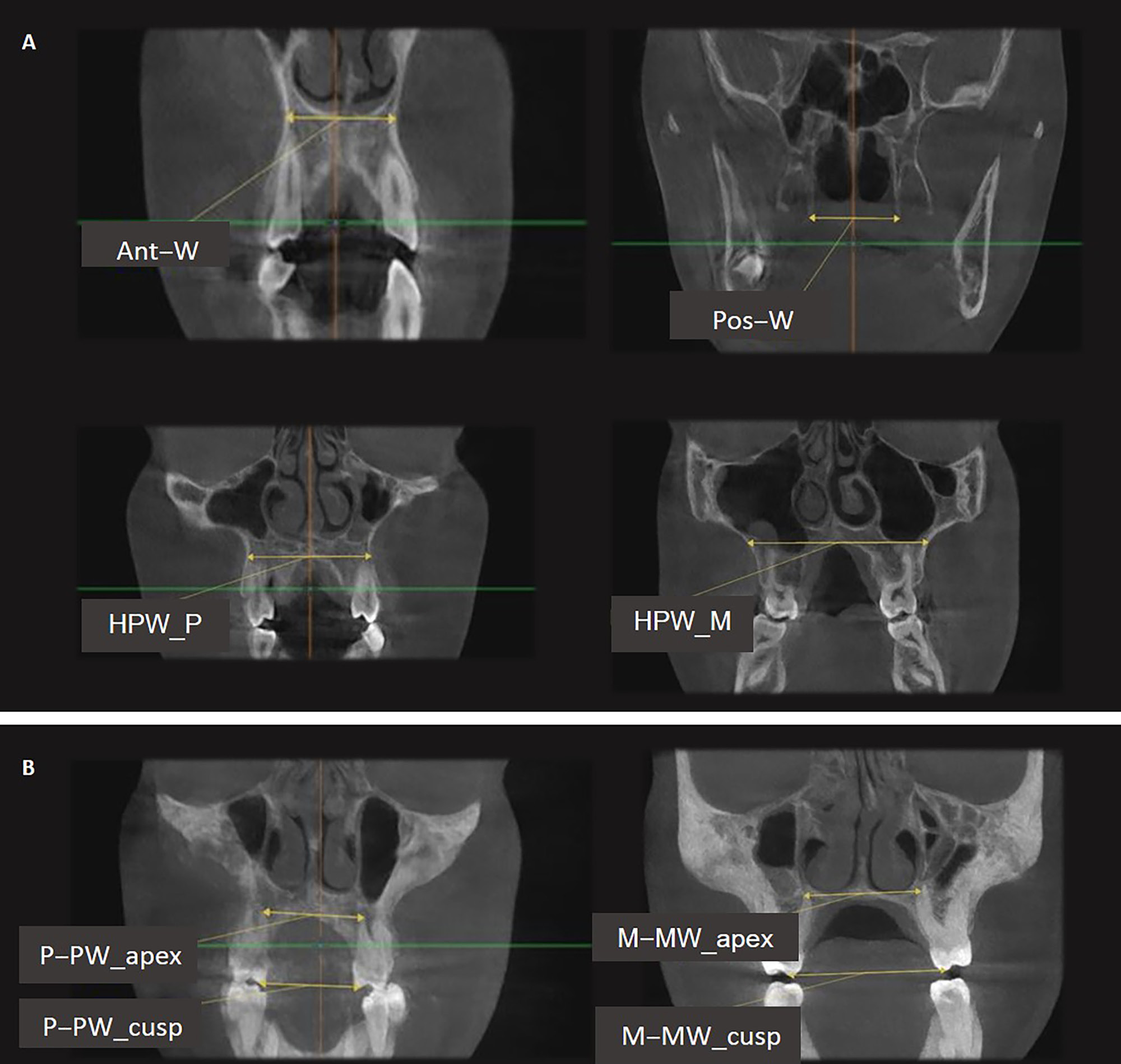
To ensure the appropriate position of the patient’s head, it was oriented in such a way that the Frankfurt plane was parallel to the horizon. The imaging system SCANORA® 3D (Soredex, Tuusula, Finland) was used (amperage: 12.5 mA; voltage: 90 kV; voxel size: 0.25 × 0.25 × 0.25 mm3; mean scanning time: 20 s). Two CBCT images were taken at the following time points: before expansion (T1); and 3 months after expansion and the removal of the appliance in the RME group, and 1 month after expansion and the removal of the appliance in the SME group (T2). Eight landmarks were identified on CBCT images: 4 skeletal landmarks (right/left pterygoideous point and right/left piriform point); and 4 dental landmarks (right/left root apex and right/left cusp tip) (Table 1).5 Four skeletal measurements were made: anterior palatal width; posterior palatal width; palatal width at premolars; and palatal width at molars (Table 1).5, 15 Six dentoalveolar measurements were made: inter-premolar width at the root apex; inter-premolar width at the cusp tip; inferred premolar tipping; molar width at the level of apices; molar width at the level of cusps; and inferred molar tipping (Table 1).5 Figure 3 and Figure 4 demonstrate the landmarks and measurements used. The definitions were derived from studies by Martina et al.5 and Lin et al.15 Both ‘inferred’ premolar and molar tipping measurements were given in millimeters (i.e., they were linear measurements), although they indirectly represented the amount of change in the buccolingual inclination of premolars and molars.5
Statistical analysis
Minitab, v.17, was used for data analysis. The normality of the distribution of each variable was checked using the Shapiro–Wilk test. Parametric tests were applied when the data was normally distributed; otherwise, non-parametric tests were employed. The two-sample t test or the non-parametric Mann–Whitney U test was used to detect significant differences between the 2 groups, whereas the paired-samples t tests or the Wilcoxon signed-rank tests were used to detect significant differences within each group.
Error of the method
Ten CBCT images were randomly chosen from the gathered CBCT images using a list of random numbers generated by the Minitab software and they were re-measured at a 1-month interval by the same principal researcher (NR). The intraclass correlation coefficients (ICCs) were used to determine the reproducibility of the employed method, i.e., intra-observer reliability (or a random error), whereas the paired t tests were used to determine any systematic error.
Results
A total of 34 patients (15 males and 19 females) were enrolled in this trial. The RME group included 17 patients (8 males and 9 females; average age: 13.76 ±0.32 years), whereas the SME group also included 17 patients (7 males and 10 females; average age: 14.02 ±0.28 years), without a statistical difference between the 2 groups regarding gender distribution (p = 0.729). No patient withdrew from the study, and therefore the total number of patients who entered the data analysis stage, in which per-protocol analysis was performed, remained 34 (Figure 1).
The descriptive statistics of the CBCT-based skeletal and dentoalveolar measurements at the beginning of treatment (T1) and at the end of the observation period (T2) in each group are presented in Table 2.
Changes in the skeletal widths
The anterior skeletal width of the maxilla increased in both groups similarly, without any significant differences between them (1.32 ±1.21 mm and 1.35 ±0.97 mm for the RME and SME groups, respectively; p = 0.926). The posterior skeletal width increased in both groups similarly, without any significant differences between them (0.49 ±0.76 mm and 0.01 ±2.49 mm for the RME and SME groups, respectively; p = 0.444). The skeletal width of the upper jaw in the premolar region increased in both groups similarly, without any significant differences between them (2.08 ±1.87 mm and 2.60 ±2.61 mm for the RME and SME groups, respectively; p = 0.511). The skeletal width change of the upper jaw in the molar region at T2 was significantly greater in the SME group as compared to the RME group (1.33 ±1.03 mm and 0.54 ± 0.37 mm, respectively; p = 0.008) (Table 3).
Changes in the dental widths
The dental width change in the premolar region at the level of apices at T2 was significantly greater in the SME group as compared to the RME group (2.16 ±2.32 mm and 0.40 ±0.88 mm, respectively; p = 0.007). No statistically significant differences between the 2 groups were found in the premolar region at the level of cusps, and in the molar region at the levels of apices and cusps (p = 0.243, p = 0.335 and p = 0.062, respectively) (Table 3).
Changes in posterior teeth tipping
The inferred tipping of premolars increased in both groups similarly, without any significant differences between them (3.80 ±2.98 mm and 3.03 ±3.08 mm for the RME and SME groups, respectively; p = 0.461). The inferred tipping of molars increased in both groups similarly, without any significant differences between them (3.72 ±2.49 mm and 5.14 ±2.53 mm for the RME and SME groups, respectively; p = 0.108) (Table 3).
Discussion
The patients included in this study were in the early permanent-dentition period (12–16 years). This age group was chosen after reviewing the medical literature, which confirmed the possibility of the expansion of the median palatal suture in this age range.16, 17, 18 Some authors have obtained successful outcomes using the conventional RME in post-adolescents and young adults up to 25 years old.19, 20 In a recent study by Jimenez-Valdivia et al., it was demonstrated that the chance of having an open midpalatal suture in patients aged 10–15 years, 16–20 years and 21–25 years was 70.8%, 21.2% and 17.0%, respectively.20 This confirmed that the expansion of the palatal suture could be effectively performed during the early permanent-dentition period (12–16 years).
In the RME group, a modified Hyrax expander was used to take advantage of the presence of posterior acrylic bite planes that prevent or limit the lengthening of the posterior teeth.21 In the SME group, a removable expander with smooth acrylic posterior bite planes was used; this appliance has been shown to be more comfortable and less painful than fixed appliances.22, 23
All patients underwent CBCT imaging before expansion and after the retention period. The retention period was necessary to ensure enough time for the midpalatal suture to gain adequate remineralization, as well as to reduce the post-expansion relapse.15
In the current study, the posterior cross-bite was effectively treated, with significant increases in most transverse widths in both experimental groups. Transverse skeletal expansion was accomplished in both groups in approximately equal amounts. Resistance to expansion appeared in the region of the pterygoid processes, where the average amount of expansion was minimal (0.49 mm and 0.01 mm for RME and SME, respectively). This change was twice and a half smaller than that noticed in a study by Martina et al., who showed an average increase in the posterior width of 1.2 mm and 0.6 mm for RME and SME, respectively.5 Differences between their findings and the present ones could be due to different age groups; in the former case, the participants were younger. While RME has been assumed to generate moderate stresses within the cranial base in children (7–11 years), other researchers have claimed that RME would probably create only sprains in the pterygoid processes of the sphenoid bone in older age.24, 25, 26
Concerning the average increases in the skeletal widths at the premolar and molar levels, and in the anterior and posterior segments in the present study, there were not any significant differences between the experimental groups except for the transverse change at the level of molars, which was greater in the SME group as compared to the RME group (1.33 mm and 0.54 mm, respectively). Although this difference was statistically significant, it can be considered clinically negligible.
The average increases in the skeletal widths in the current study were 2–3 times smaller than those reported in studies by Martina et al.5 and Lanteri et al.27 The reason for such differences is probably the younger age of patients in these 2 studies, which could be associated with more efficient bone metabolism and a more active remodeling process.28 In the current study, the mean changes in the skeletal widths increased gradually from the posterior to anterior regions, which indicated that expansion occurred along the midpalatal suture in a V-shaped pattern in both groups. It is in opposition to the homogenous pattern of expansion noticed in Martina et al.’s study.5 The difference may be attributed to the different types of devices used. In the current work, the rapid maxillary expander contained acrylic parts that tightly rested on and around the posterior teeth at both the vestibular and palatal sides; besides, the slow maxillary expander included a palatal acrylic plate that had adequate tissue contact and was supported with posterior occlusal acrylic coverage. These acrylic parts may have ensured the delivery of satisfactory force on the teeth and the palate. In contrast, Martina et al. used a two-band palatal expander, which may have applied force on bone rather than on the teeth.5 Another reason for this difference may be the older age of patients in the present study, which could be accompanied by resistance to expansion in the posterior region more than in the anterior region, giving V-shaped pattern expansion.20, 25
For dental changes, increases in all dental widths at the level of molars and premolars were noticed, with no statically significant differences between the 2 groups except for the width between the apices of premolars. The mean width change in the premolar region at the level of apices was 0.40 mm in the RME group and 2.16 mm in the SME group. This change was 5.4 times greater in the SME group. This could be explained by a longer period of SME, which may have allowed adequate time for root movement in the buccolingual direction. These amounts of dental changes differed from those reported in 2 previous studies,29, 30 which could be due to variations in the average force applied, the type of device used and the patients’ age in each study. Nevertheless, by comparing the mean amounts of dental expansion in the premolar region in the SME group, it was found that the mean increase in width at the level of cusps was 2.4 times greater than at the level of apices (5.13 mm and 2.16 mm, respectively), which meant that a buccal tipping of premolars occurred.
Buccal tipping was a common side effect of using expansion appliances. Both the RME and SME groups showed considerable changes in the tipping amounts. For upper first premolars, the average increase of tipping was a little smaller in the SME group, but the difference between the 2 groups was not statistically significant (3.80 mm and 3.03 mm for the RME and SME groups, respectively). At the same time, the mean values for the tipping changes of upper first molars were 3.72 mm in the RME group and 5.14 mm in the SME group, with no statistically significant difference between the 2 groups (p = 0.108). Similar results were found in studies by Garib et al.29 and Lin et al.15 In contrast, the values were lower in studies by Boysen et al.31 and Erdinç et al.32 These differences in dental tipping between the studies could be attributed to variations in the average force applied, the strength direction, the thickening of the alveolar bone around the roots, and the nature of the bone.
No critical harm was observed or documented in the current trial. In the RME group, patients experienced some pressure on the alveolar processes of the upper posterior teeth and in the nasal floor region during the active period of expansion, but it was well tolerated in general. In both groups, appliance fractures were found in 1 or more items of the expander during the treatment period in 4 patients (2 appliances in the RME group and 2 appliances in the SME group), which meant that the percentage of fractures was approx. 12% in each group. All fractured appliances were fixed within less than 24 h.
Limitations
Despite adherence to the calculated sample size, the number of patients was relatively small, and it is preferable to increase the number of patients in future research work to get more powerful statistical results. The current two-arm study compared RME with SME, and there was no an untreated control group. If a three-arm study design had been followed, we would have been able to compare the outcomes between the 3 groups by filtering out the growth effects and observing any possible spontaneous improvement of posterior skeletal maxillary constriction. Patients’ responses, the levels of discomfort and pain, as well as quality of life should be assessed in future research work. This study did not assess the changes in the dimensions of the upper airways following maxillary expansion, and this aspect should be considered in future clinical trials. From a methodological perspective, the blinding of patients and care providers was not possible due to the nature of the interventions. This might be a source of detection bias. Since the current analysis of maxillary changes referred to a relatively short time, long-term follow-up periods to detect any post-retention relapse should be taken into account in future trials.
Generalization
The results of the current work could not be generalized to other kinds of expanders or the same types of expanders with different activation protocols. Therefore, more future clinical research with a larger number of patients and longer follow-up periods is required.
Conclusions
Slow maxillary expansion can be an effective alternative to RME in the early adolescence period (12–16 years). The average increases in the skeletal and dental widths were approximately similar in both groups except for skeletal expansion at the level of upper molars and dental expansion at the level of the apices of upper premolars, which were greater in the SME group. Furthermore, the buccal tipping of premolars and molars was observed as a side effect in both groups.
Trial registration
The trial was retrospectively registered at ClinicalTrials.gov (ID: NCT03667508).
Ethics approval and consent to participate
The study was approved by the institutional Research Ethics Committee at the University of Damascus, Syria (UDDS-2675-15,032,017/SRC-4771). Written informed consent was obtained from all participants.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.