Abstract
Background. The success of periodontal surgery depends on the appropriate coaptation of the incised edges, the elimination of empty spaces and the reduction of the amount of blood coagulum. In free gingival graft (FFG) surgery, the stabilization of the graft, hemostasis and cleansing the site remain a necessity.
Objectives. The aim of the present study was to compare the use of the tissue adhesive N-butyl cyanoacrylate + octyl cyanoacrylate (N-BCA + OCA; Iceberg-glue®) and surgical sutures to evaluate the stabilization and fixation of FGG, which is indicated to increase the width of the keratinized attached gingiva.
Material and methods. A total of 24 cases – 12 patients aged 18–45 years with gingival recession and the absence of the keratinized gingiva underwent FGG surgery at 2 parallel sites at the same time. A long piece of FGG was taken from the palate, from the area adjacent to a canine to a second molar, and divided into 2 equal pieces. The bed of the graft was prepared at each side with a 15C blade. One piece was applied to each bed, one graft was sutured using 0/5 nylon sutures and the other one was stabilized using the tissue adhesive.
Results. The data analysis showed that the postoperative pain ended after 3 days at the tissue adhesive site, but it continued up to 4 days at the suture site. The healing index was significantly better after 2 months at the tissue adhesive site. Graft shrinkage was significantly lower after 3 months at the tissue adhesive site, whereas there was no significant difference in graft shrinkage between the 2 methods at 6 months after the surgery.
Conclusions. The Iceberg-glue tissue adhesive proved to be a reliable alternative material to sutures in stabilizing the free gingival graft at the recipient site. It reduced postoperative pain and improved the healing of the recipient site.
Keywords: tissue adhesive, cyanoacrylate, free gingival graft, keratinized attached gingiva
Introduction
The survival of a free gingival graft (FGG) depends on multiple factors, including the appropriate coaptation of the incised edges, the avoidance of any empty spaces and the reduction of the amount of blood coagulum. In FGG surgery, the stabilization of the graft, stopping the bleeding and cleansing the bed of the graft remain a necessity.1 Sutures are the most popular technique for the appropriate coaptation of the graft; however, new materials and mechanisms are being studied in order to achieve and maintain the stability of the graft in its bed, and to prevent the invasion of any foreign bodies.2, 3 Using cyanoacrylate tissue adhesives in FFG surgery, has proved to be easy and effective, and it also causes fewer problems as compared to the use of sutures. In addition, due to their antibacterial properties, tissue adhesives decrease the risk of a toxic effect.4, 5
Free gingival grafting, introduced in 1968,6 is a routine clinical procedure in oral surgery. The inadequate amount of the attached gingiva presents a big surgical problem. In addition, it does not allow patients to control plaque effectively. The localized gingival inflammation at a specific site is considered as a sign of the insufficient width of the attached gingiva, regardless of the overall satisfactory oral hygiene. The novel clinical and histological research suggests that any width that allows the maintenance of healthy periodontium can be regarded as sufficient.7
Free gingival grafting is commonly utilized to increase the width of the attached gingiva.8 It is considered as the gold standard in this regard due to its autogenous character, the ease of technique and the possibility of maintaining of the keratinized tissue. In addition, in case of FGG, surgical outcomes can be predicted.9
Different amounts of graft shrinkage have been noticed during the healing period.10, 11 The permanent nutrition of the graft affects graft shrinkage; there must not be any factors that disrupt the continuity of graft nutrition. As stated by Sullivan and Atkins, the thickness of the graft, an atraumatic surgical procedure and the rapid fixation of the graft are essential for preserving graft vessels from any harm and dehydration, thereby minimizing the chances of shrinkage.6 Accordingly, the number of sutures should be decreased to minimum, since every suture induces a localized hematoma under the graft, which may increase graft shrinkage. For that reason, the sutureless stabilization techniques might help to minimize or even prevent graft shrinkage; adhesives might be an appropriate method to achieve this target.11
Tissue adhesives were introduced for the first time as an alternative to sutures by Ardis in 1949.12 The performance of cyanoacrylate tissue adhesives was examined by Coover et al. in 1959; it was chemically analyzed and suggested for application in surgical procedures.13 Tissue adhesives were employed in the early 1960s, but unluckily, the resultant inflammatory reactions were not acceptable. Therefore, many modifications have been made to minimize their unfavorable inflammatory effects. Other problems related to the use of tissue adhesives were the lack of good training and the incorrect use resulting from by the insufficient knowledge in this field.
Several types of tissue adhesives have been developed and improved due to continuous research and technological development, and they have been approved and licensed by the U.S. Food and Drug Administration (FDA).14
Cyanoacrylates are a type of tissue adhesives that have been developed 50 years ago to repair injuries.15 In 1974, Binnie and Forrest compared butyl cyanoacrylates and silk sutures in the stabilization of periodontal flaps, and they found lesser edema and swelling as well as a better gingival contour in the butyl cyanoacrylate group.16
Free gingival graft surgery was done for the first time without the use of any sutures by Hoxter in 1979.1 He thought that the graft could survive without any sutures only if it had been positioned and fixed at the recipient site correctly. He postulated that it was possible to obtain the intended stability, sterility, and even homeostasis.1
N-butyl cyanoacrylate + octyl cyanoacrylate (N-BCA + OCA) (Iceberg-glue®; GMI, Barcelona, Spain) is a new combination of tissue adhesives, manufactured by blending 2 different kinds of cyanoacrylate, giving the adhesive better flexibility, while keeping high levels of resistance. Actually, scientific literature illustrates that N-BCA is a cyanoacrylate molecule with the highest tensile strength (34.27 N) and low flexibility.17 On the other hand, OCA has a lower tensile strength (11.27 N) and at the same time it has better elastic features. The Iceberg-glue adhesive has an excellent tensile strength, in addition to good elasticity due to the presence of OCA. In addition to the abovementioned characteristics, this formula has hemostatic, sealing, antibacterial and adhesive properties. Polymerization starts about 2 s after the application and is completed after 60 s. The temperature generated during the polymerization process is about 45°C,18, 19 which is lesser than for other kinds of cyanoacrylates.20, 21 The intraoral use of tissue adhesives is limited to superficial application.22 Cyanoacrylate tissue adhesives keep their adhesive properties even in the presence of humidity.23
There are not enough studies that have aimed to evaluate wound healing and assess patient-centered outcomes. The aim of this study was to compare patient-centered outcomes, postoperative pain, wound healing, and the shrinkage of FGG between two recipient sites – one fixed with sutures and the other with cyanoacrylate tissue adhesives.
Material and methods
Trial design
This study is a two-arm, split-mouth, randomized controlled clinical trial comparing a tissue adhesive (Iceberg-glue) and surgical sutures with regard to the levels of pain, the modified early-wound healing index (MEHI) and the shrinkage of the graft.
This randomized clinical trial (RCT) was approved by the institutional Ethics Committee at the Faculty of Dental Medicine of the University of Damascus, Syria (No. 2773MS). The protocol was registered in the ISRCTN registry (ISRCTN10301784).
Our study recruited patients who were referred to the Department of Periodontology, Faculty of Dental Medicine, the University of Damascus, between April 2019 and June 2019. The procedure was fully explained to all patients and written informed consent was obtained from them.
Sample size
The G*Power software, v. 3.1.7 (https://www.psychologie.hhu.de/arbeitsgruppen/allgemeine-psychologie-und-arbeitspsychologie/gpower), was used to calculate the sample size with an alpha level of 0.05 and a power of 80 (based on previous research24); a sample size of 24 cases was required (12 patients).
Eligibility criteria
All patients who required FGG surgery to increase the amount of the keratinized tissue at 2 parallel sites, i.e., had the attached gingiva lower than 1 mm, were considered as eligible candidates for our study.
Those who were older than 18 years, and had the plaque score and the bleeding score <20% were enrolled. Patients with uncontrolled diabetes or coagulation disorders (with liver disease, on the anticoagulative therapy, etc.), those who took corticosteroids, or had any systemic disorder that would disturb oral and periodontal surgery were excluded. Figure 1 illustrates the process of recruitment.
Allocation concealment
The patients were asked to choose a sealed envelope to decide which site was going to be stabilized with sutures and which one with the tissue adhesive. The envelopes were unsealed just before the surgery. The follow-up measurements were done by another dentist (W.A) who did not have any information regarding our current trial.
Description of the intervention
This RCT was done on 24 cases – 12 patients aged between 18–45 years who had an insufficient amount of the attached gingiva and FGG was recommended.
All patients underwent an initial periodontal therapy that consisted of providing oral hygiene instructions, motivating, scaling, polishing, and root planing if necessary. All patients were examined at baseline and 2 months after the completion of the initial periodontal treatment to determine if there was a necessity to increase the width of the attached gingiva or not. The plaque and bleeding scores in the whole mouth were <20% at the recall visit.
One long piece of the graft was harvested from the palate, from the area between a second molar and a first premolar; then, it was divided into 2 equal parts and the thickness of the graft was standardized between the 2 sides, as the graft thickness is an important factor affecting the shrinkage of the graft.6
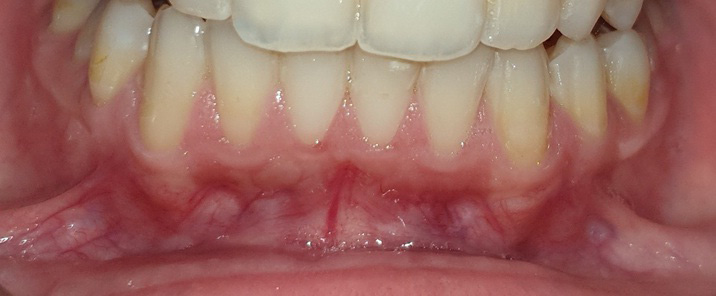
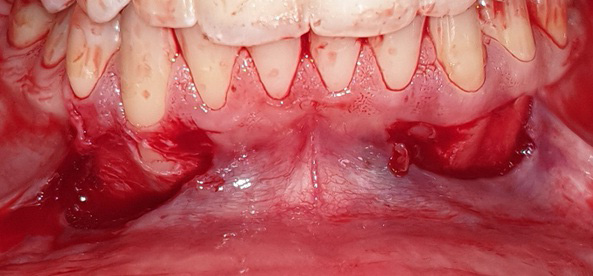
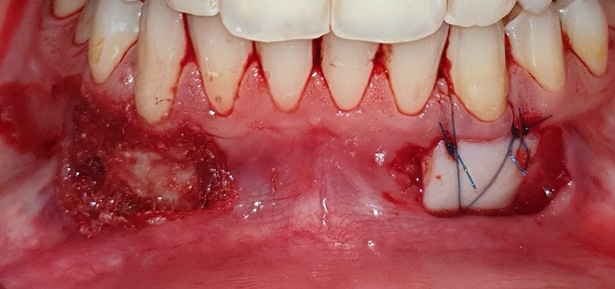
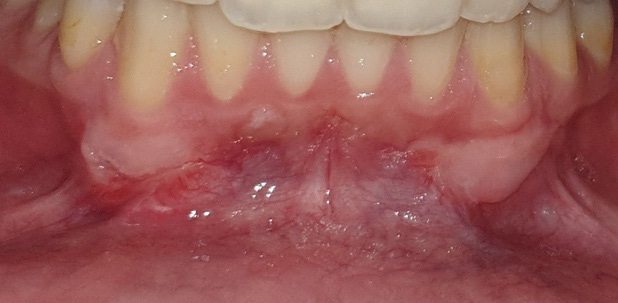
The graft was positioned in its bed and held pressed for 2 min for initial stability. At one side, the graft was stabilized using 0/5 nylon sutures (interrupted sutures to the papilla and a sling suture were placed to adapt the graft intimately to the root and periosteal bed),25 while at the other side, FGG was stabilized with the tissue adhesive (Figure 2, Figure 3, Figure 4).
The blood supply between FGG and the recipient site is essential for the healing process, as well as atraumatic graft fixation for the maintenance of plasmatic circulation.24
Outcomes and follow-up
The primary outcome was the shrinkage of the graft, which was assessed at 2 months, 3 months and 6 months after the surgery. The length and width of the graft were measured using the University of North Carolina-15 (UNC-15) periodontal probe. The secondary outcomes were the recipient site healing and the recipient site pain.
The recipient site healing was assessed by means of MEHI26 at 1 week, 2 weeks, 1 month, and 2 months after the surgery. The healing progress was evaluated using the Landry, Turnbull and Howley healing index, which classifies healing on the basis of redness, and the presence of bleeding, granulation tissue, epithelialization, and suppuration, and rates it from score 1 (very poor healing) to 5 (excellent healing) accordingly.27
The recipient site pain was assessed by the patient with the use of a 1–10 visual analog scale (VAS).28 A questionnaire sheet was given to the patients to document the levels of pain from the recipient site before taking any analgesics at 6 h, 12 h, 24 h, 2 days, 3 days, 4 days, 5 days, 6 days, and 7 days after the surgery.
Analgesics were taken only when needed (ibuprofen 500 mg, PRN), a mouth rinse (chlorhexidine 0.12%) was prescribed twice a day for 1 week, and instructions were given to avoid eating any solid or hot food in the 1st week after the surgery. The patients were also instructed to return 1 week after the operation to remove sutures and to bring the questionnaire sheet.
Statistical analysis
The data analysis was carried out by means of the SPSS Statistics for Windows software, v. 17.0 (SPSS Inc., Chicago, USA), using a two-tailed test with alpha set at 0.05. Descriptive statistics were reported as mean and standard deviation (M ±SD) for continuous variables, and as frequency and percentage (n (%)) for categorical variables.
The data was analyzed at baseline and during the postsurgical follow-up with parametric tests, when the variables were distributed normally. To evaluate ordinal variables, non-parametric tests were implemented; the Mann–Whitney U test when the 2 variables were not related, while the Friedman and Wilcoxon tests declared that differences within the same variable were checked across multiple time points. The required assumptions for each of the aforementioned tests were insured before conducting them.
Results
12 patients (24 cases) were recruited from the start and were eligible for analysis. Their mean age was 27.0 ±8.4 years. The percentage of females was 75% (n = 9). The patients’ baseline characteristics are shown in Table 1. A single calibrated examiner (W.A) did all measurements. There was no significant difference between the study groups at baseline in terms of gender, age and graft site.
The size of the graft reduced significantly within the 2 groups at 2, 3 and 6 months after the surgery (p < 0.05). After 2 and 6 months, there were no significant differences between the 2 groups. However, after 3 months, the cyanoacrylate group showed significantly less shrinkage as compared to the other group (p < 0.05) (Table 2).
The VAS score at the recipient site decreased from day 1 and reached a nadir at day 3 in the tissue adhesive group, while the same pain nadir level was achieved on day 4 in the suture group. Table 3 and Table 4 depict the pain scores in different groups.
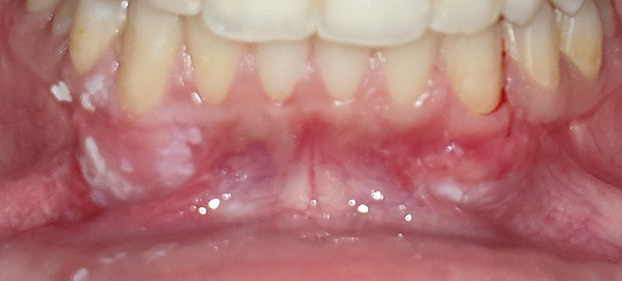
As to the healing index, there were no significant differences between the 2 sites after 1 week, 2 weeks, 1 month, and 2 months. However, the healing process was completed 1 month postoperatively in the tissue adhesive group, whereas in the suture group, it lasted up to 2 months (Table 5) (Figure 5, Figure 6, Figure 7).
Discussion
In the present RCT, the use of a tissue adhesive and surgical sutures, two different graft stabilization techniques, were compared in terms of recipient site postoperative graft shrinkage, pain levels and healing index (MEHI). Our main findings were that there was no significant difference in graft shrinkage, but the pain levels were significantly lower and healing was significantly better at the tissue adhesive site.
After 3 months, at the cyanoacrylate side, graft shrinkage was significantly lower than at the other side with surgical sutures (p < 0.05); however, there was no significant difference between the 2 sides observed at 2 months and the difference disappeared at 6 months after the surgery. It might be attributed to the fact that there was no or very little trauma caused to the bed of the graft at the 2 sides while operating. Our findings are supported by a study conducted by Barbosa et al., who fixed FGG with ethyl cyanoacrylate in one group and with silk mucoperiosteal sutures in the other.24 The mean graft area measured in square millimeters on day 30, day 45 and day 90 was 60.9 ±15.1, 54.5 ±16.1 and 54.5 ±16.1 in the cyanoacrylate group and 59.0 ±2.4, 57.1 ±1.3 and 57.1 ±1.3 in the suture group, respectively. No significant difference was found between the study groups for alterations in the grafted area.24 On the contrary, Paknejad et al. observed a significant difference in graft shrinkage 3 months postoperatively after stabilizing FGG with a tissue adhesive and silk sutures.29 Similarly, Gümüş and Buduneli, who compared the traditional technique, the use of a cyanoacrylate tissue adhesive or microsurgery in terms of graft stabilization, observed that graft shrinkage was significantly lesser at the cyanoacrylate site than at the other two.30 The proposed explanations were that a shorter and atraumatic operation in the cyanoacrylate group along with the soft pressure applied to the graft before it was stabilized in its bed had a significant role in maintaining avascular plasmatic circulation, which eventually results in less shrinkage.
The VAS score indicted no pain at the recipient site 3 days postoperatively in the tissue adhesive group, but the pain lasted for 4 days in the suture group. Since graft stabilization with a tissue adhesive appeared in a considerably shorter time, less inflammation and edema were expected; hence, lower postoperative pain. This might explain why the tissue adhesive sites became pain-free rapidly. Zucchelli et al. found that a longer operative time in the control group may have balanced the secondary intention wound healing experienced by the test group in terms of pain in the postoperative period.31 Paknejad et al. found no significant differences in pain levels between the 2 groups.29 The contradiction between our findings and those of Parkenjad et al. might be due to the difference in the chemical composition of the tissue adhesives used.
One of the important issues in FGG surgery is the graft and recipient site healing. We found that the tissue adhesive significantly reduced the time needed for healing the wound and accelerated wound healing. Approximately, we achieved complete wound healing at the tissue adhesive side after 1 month. On the other hand, a 2-month period was needed for complete wound closure at the suture side. Paknejad et al. found a significant difference between the 2 groups in the healing process after 10 days, though there were no significant differences in the healing process after 20 and 90 days.29 It might be due to the fact that they used an ethyl 2-cyanoacrylate-based tissue adhesive; the component is short-chained and rarely used, as it degrades very rapidly and allows for the subsequent formation of formaldehyde, which is very toxic.32
Strengths and limitations
Our study was the first RCT to evaluate the new brand of cyanoacrylate-based tissue adhesive for the oral mucosa (Iceberg-glue), comparing it with the classical way of suturing. Since it was difficult to blind the sites from the dental surgeon, we implemented a strict protocol to insure that the outcome analyzers were blinded to the sites, using an objective way of assessment. However, our study has some limitations. For example, the assessment of pain scores and some of the questionnaires were subjective in nature. In addition, due to the limited resources, we were not able to recruit more patients, despite efforts to do so, in order increase our sample size.
Clinical significance
A tissue adhesive could be a reliable alternative material to sutures in stabilizing FGG at the recipient site. It reduced postoperative pain and improved the healing of the recipient site.
Conclusions
In this study, whether the grafts were fixed with N-butyl cyanoacrylate + octyl cyanoacrylate (N-BCA + OCA) or nylon sutures, differences in graft size were not statistically significant. Also, this study suggests that the N-BCA + OCA tissue adhesive is capable of accelerating and boosting the healing of gingival tissue wounds. Further research with longer follow-up periods on tissue adhesives is needed, as postoperative pain was significantly lower at the tissue adhesive site (it ended after 3 days at the tissue adhesive site and after 4 days at the suture site). Therefore, the use of cyanoacrylate may be a promising alternative for the conventional technique to stabilize free gingival grafts.
Trial registration
The trial was registered at the ISRCTN registry (ISRCTN10301784).
Ethics approval and consent to participate
The study was approved by the institutional Ethics Committee at the Faculty of Dental Medicine of the University of Damascus, Syria (No. 2773MS). Informed written consent was obtained from all the patients.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.