Abstract
Background. Fixed implant-supported restorations are mainly used in dental implantology. In comparison with screw-retained implants, cement-retained prostheses have the following advantages: the ease of splinting implants; increased passive casting; and procedural similarity to conventional tooth-supported fixed partial dentures. Furthermore, they show reduced fracturing of components with better esthetic outcomes and an improved force direction, along with a reduced cost and less chairside time.
Objectives. The aim of this study was to evaluate the effect of different geometric changes in the dental implant abutment body on the amount of residual excess cement (REC) and the retention of cemented implant-supported prostheses.
Material and methods. Seventy-two straight abutments were categorized into 4 groups: vertical groove; 1 horizontal groove; 2 horizontal grooves; and ccontrol (with no geometric changes in the abutment). The access hole was partially filled and the cast copings were cemented using Temp-Bond™ NE, a non-eugenol cement. The difference in weight before and after removing the excess cement was considered as REC. Furthermore, the retention of the cast coping was measured as the force that was required to separate the cemented cast coping from the abutment.
Results. The mean REC values of the groups with 1 and 2 horizontal grooves were significantly different as compared to the control group (p < 0.05).
Conclusions. This study shows that the presence of 1 or 2 horizontal grooves in the abutment body significantly reduces the amount of REC in comparison with control.
Keywords: dental implants, cement, abutment type
Introduction
Implant-supported fixed dental prostheses are a good treatment choice, which has developed into a standard of care in dentistry. This achievement may be due to the osseointegration process and the improved stability of the interfaces between the implants, the abutments and the dental prosthesis.1 Fixed implant-supported restorations are usually retained on abutments with screws or cement.2 Both abutment types have their own benefits and drawbacks. It is the clinician’s responsibility to decide on the most suitable technique for each individual case.1 A recent systematic review found that the retention type (cement or screws) might not have a critical effect on the general survival of the prosthesis, but rather was responsible for the development of certain complications.3 In comparison with the screw-retained type, cemented prostheses have the following advantages: the ease of splinting implants; increased passive casting; and procedural similarity to conventional tooth-supported fixed partial dentures.4 Additionally, they show reduced fracturing of components with better esthetic outcomes and an improved force direction, along with a reduced cost and less chairside time.2, 5, 6 Investigators have concluded that the cement retention method is preferred over the screw-retained abutment type in the following cases: short-span prostheses with margins at or above the mucosa level; inappropriately inclined implants; and narrow-diameter crowns.1
The main disadvantage of cemented prostheses is residual excess cement (REC), which can cause the inflammation of soft tissues around the implant.7, 8 Multiple research studies have shown that REC around the implant can result in a rough surface and facilitate plaque accumulation, and consequently damage soft tissues around the implant due to bacterial colonization.6 Several techniques have been proposed to reduce the amount of REC, such as minimizing the amount of cement used,9 creating a vent hole,9, 10 using cements of higher viscosity, applying modified cementation methods, or the selective removal of the abutment walls.11, 12
Changing the design of the abutment body is another method explored in some studies.6, 13 Various modifications in the geometric design of the abutment body have been investigated, like the creation of a vent hole or a groove. Such changes made to the abutment body can act as an internal vent that may reduce REC.6, 8
Unreliable retention is another concern about cemented restorations.14 To circumvent this drawback, the following methods to increase the retention rate have been proposed: changes in the abutment surface texture; modified cementation methods; and the selective removal of the abutment walls.13, 14 The abutment surface can be changed by creating grooves. Such changes can reduce REC and improve the retention of the prosthesis.12
Objectives
The aim of the present study was to investigate how different geometric changes in the dental implant abutment body influence the amount of REC and the retention of cement-retained implant restorations. The null hypothesis stated that all of these modifications could reduce REC and increase the retention of cement-retained implant restorations.
Material and methods
Abutment modification
The sample size was calculated with the Power and Sample Size Calculator (PS) software, v. 3.1 (https://ps-power-and-sample-size-calculation.software.informer.com/3.1/) as 13 samples per group (n = 13). This was based on the results of a study by Wadhwani et al.,6 with α = 0.05 and a power of 80%. To increase the validity of the study, 18 samples were considered for each group, resulting in a total of 72 samples. The straight abutments (OSSTEM®; Osstem Implant, Busan, South Korea) used in this study were 5.5 mm in length, 4.5 mm in diameter and 1 mm in gingival height.
Coping fabrication
In order to mold the coping crown, the access holes of the abutments were carefully blocked out with wax during the laboratory procedures. For uniformity between the study groups, a three-dimensional (3D) printer was used to design the coping patterns. Since the abutments were similar prior to implementing the changes, one of the abutments was scanned using a Maestro® 3D scanner (AGE Solutions, Pontedera, Italy), and then designed with the Exocad software (Exocad, Darmstadt, Germany), considering a cement space relief of 50 μm. After that, the scanned and designed copings were made with a 3D printer (Prodent® 3D printer; Bonyan Mechatronic, Tehran, Iran) and a light-curing moldable 3D resin (Freeprint® cast; Detax, Ettlingen Germany), and casted with base metal alloys (Sankin®, non-beryllium; Dentsply Sirona, Tokyo, Japan). The cast copings were examined under an optical microscope (Nikon, Tokyo, Japan) at ×20 magnification to assist in adaptation to their corresponding abutments and any irregularities were removed with a milling round of ½. A vertical mark was created on the copings in the corresponding area of the flat side of the abutments to guide the placement of the copings on the abutments.
The abutments were tightened with the ratchet of the OSSTEM system by using a torque of 25 N·cm on the fixture analogs of the same system and mounted in acrylic blocks to help with the operation. Each of the 4 study groups contained 18 individual abutments with the indicated modifications. In group 1, each abutment had a vertical groove measuring 0.5 mm × 0.5 mm from the occlusal surface of the abutment up to 1 mm above the finish line; it was created with a bur (KaVo Dental, Biberach, Germany). Each abutment of group 2 had a horizontal groove (0.5 mm × 0.5 mm) that was created at a distance of 3 mm from the occlusal edges. The abutments of group 3 had 2 horizontal grooves (0.5 mm × 0.5 mm) with a 1-millimeter distance. The control group (group 4) consisted of 18 abutments with no changes in the abutment body.
Cementation
Before cementation, the abutment screw access channel was filled up to 1 mm on the occlusal surface with Coltosol® (Coltène/Whaledent, Altstätten, Switzerland). To measure the amount of REC, the weight of coping/abutment/analog/acrylic block was determined with an A&D scale (EK-300i; A&D Company, Tokyo, Japan). A dental cement (Temp-Bond™ NE; Morris Dental Company, Dublin, Ireland) was mixed according to the manufacturer’s instructions and applied to the intaglio surface until the coping was filled in approx. 75%. The weight of coping/abutment/analog/acrylic block with cement was then measured before placing the coping on the abutment. Next, the copings were placed – initially by finger pressure – on the mounted abutments, followed by a pressure of 5 kg for 7 min with a universal testing machine (model HSK-S; Hounsfield Test Equipment, Redhill, UK). The excess cement was then removed with a plastic scaler and coping/abutment/analog/acrylic block was weighted again after cleaning (Figure 1).
REC evaluation
The following formula was used to measure REC (Equation 1):
Evaluation of retention
The samples were then incubated at 37°C and 100% relative humidity for 24 h. The specimens were assembled in a universal testing machine and subjected to a pull-out test (retention) at a crosshead speed of 1 mm/min. The force required to remove the copings was recorded in newtons (Figure 2).
Statistical analyses
Data was analyzed using descriptive statistical methods (mean (M) ± standard deviation (SD)), and then compared between the groups. The normality of data was analyzed with the Kolmogorov–Smirnov test. Statistically significant differences between the studied groups in the mean REC values were investigated with the Kruskal–Wallis test. Statistically significant differences between pairs of groups were analyzed using the Mann–Whitney U test. The statistical analyses were carried out by means of the SPSS Statistics for Windows, v. 17.0 (SPSS Inc., Chicago, USA), and a p-value <0.05 was considered statistically significant.
Results
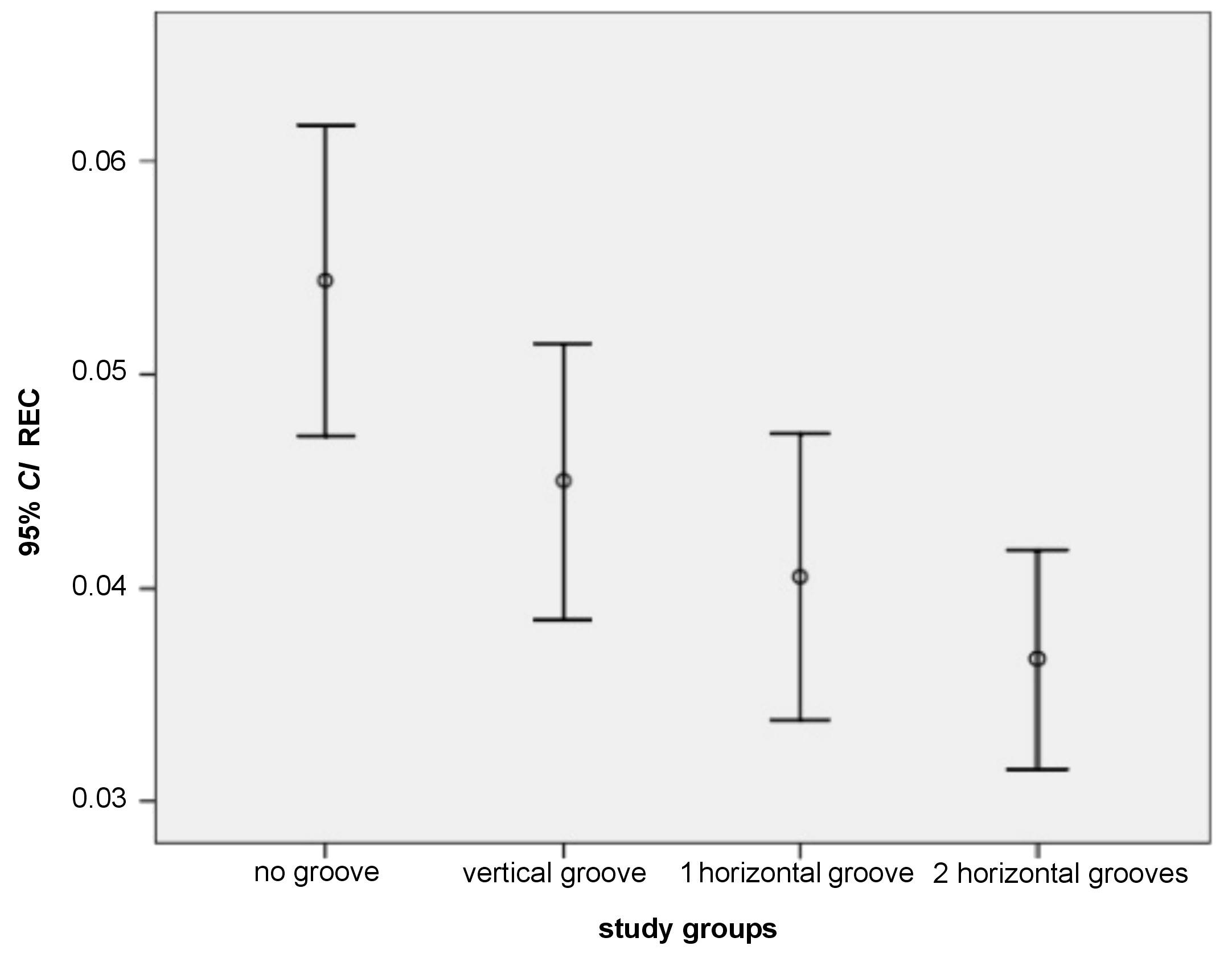
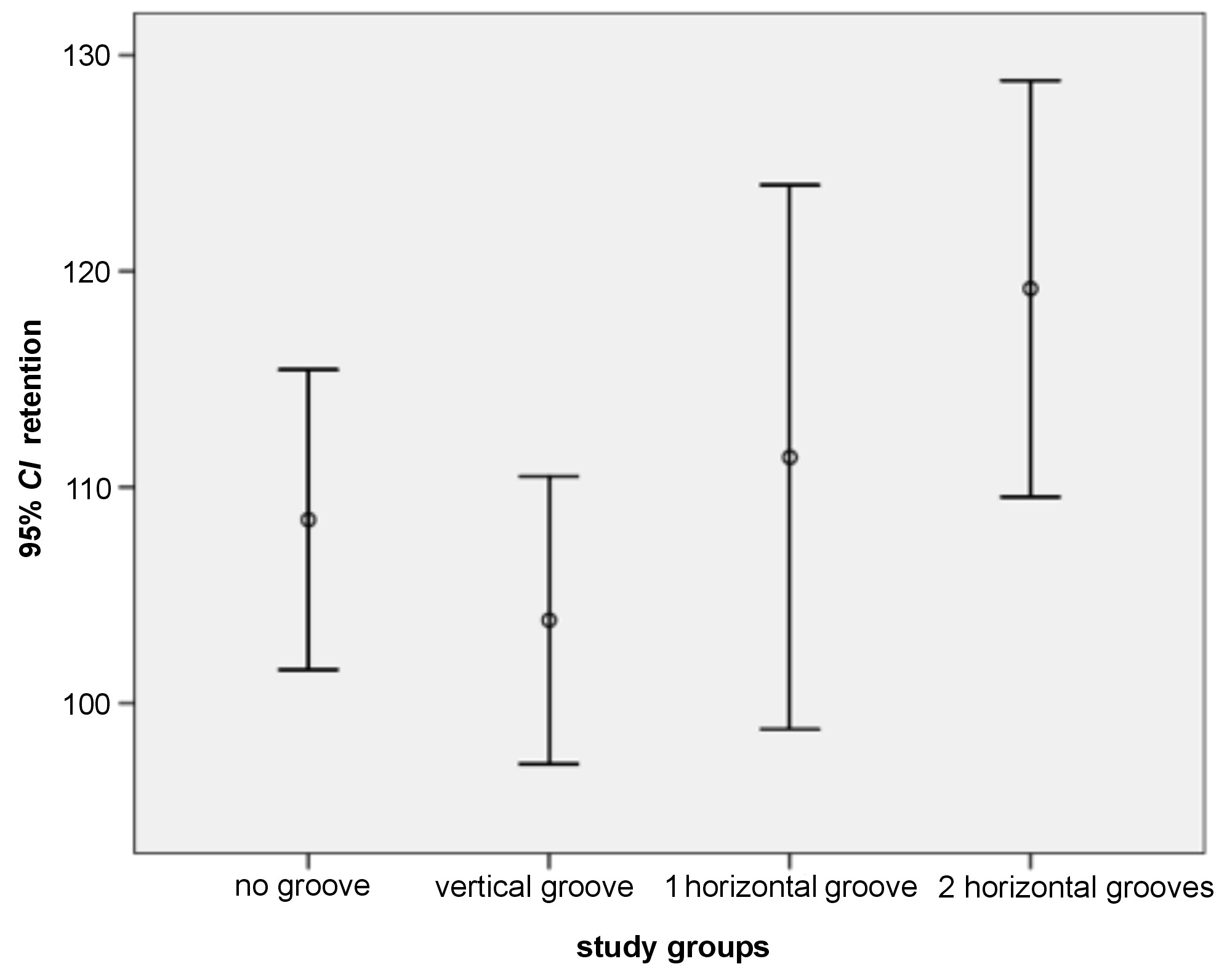
The M and SD values for the 2 variables – REC and retention – in the study groups are presented in Table 1. We found that the mean REC value was the highest in the ‘no groove’ control group. Group 3 (2 horizontal grooves) showed the lowest mean REC value. The mean retention value was the highest in group 3 (2 horizontal grooves)and the lowest in group 1 (vertical groove).
The normal distribution of the 2 variables – REC and retention – was analyzed using the Kolmogorov‒Smirnov test and we found that the distribution of the REC variable was not normal; therefore non-parametric tests were used to examine the associated hypotheses (p < 0.05). Additionally, we found that the distribution of the retention variable was normal, and therefore parametric tests were used to examine the associated hypotheses (p < 0.05). Figure 3 shows REC for the study groups and Figure 4 shows retention for the study groups. To examine if there was any statistically significant difference between the studied groups in the mean REC values, the Kruskal‒Wallis test was used. The results showed a statistically significant difference in the REC means between the study groups (p < 0.05) (Table 1). The Mann–Whitney U test was then used to compare the groups with each other; the results are presented in Table 2. There were statistically significant differences in the REC means between the ‘no grooves’ control group and groups 2 and 3 – with 1 and 2 horizontal grooves, respectively. The mean REC value in the ‘no grooves’ group was higher than the means in those 2 groups (p < 0.05). The mean REC value in the ‘vertical groove’ group was significantly higher as compared to the group with 2 horizontal grooves (p < 0.05). There were no statistically significant differences in the REC means between other study groups. To test any statistically significant difference in the mean retention between the study groups, the one-way analysis of variance (ANOVA) was used. There was no statistically significant difference in the mean retention between the study groups (Table 1).
Discussion
Implant treatment can be a challenging clinical condition, which requires a high level of communication between the surgeon, the technician and the restoring dentist.15, 16 Today, cement-retained implant-supported prostheses are widely used. However, they might have disadvantages in comparison with screw-retained ones, including REC and unreliable retention after cementation. The present study aimed to introduce modifications in the abutment that would address these problems.17, 18, 19
The main disadvantage of cement-retained implant-supported prostheses is REC, which can cause the inflammation of soft tissues around the implant.5, 7, 8 Various studies have shown that REC around the implant may result in a rough surface and facilitate plaque accumulation, and damage soft tissues around the implant due to bacterial colonization.5, 7 A cohort study found that the direct cause of damage in 80% of the soft tissues surrounding the implant was due to the colonization of bacteria on the excess cement.6 For this reason, numerous studies have investigated methods that reduce REC.
In this study, the null hypothesis about the effect of the changes made in the abutments on the amount of excess cement was rejected, and we found that only the addition of horizontal groove(s) to the abutment body resulted in reduced excess cement. On average, the amount of excess cement in the group with 1 horizontal groove was 0.0406 gr, while it was 0.0367 gr in the group with 2 horizontal grooves. Both values were statistically significantly different as compared to the control group (0.0544 gr; p < 0.05). We propose that perhaps horizontal grooves act as a reservoir and because of the circumferential shape around the abutment, they house some excess cement during the insertion of the coping. However, a vertical groove is created only in a specific area, and its function is limited and localized. Additionally, the groove might facilitate cement exit before filling the superior space of the screw hole.
Based on the reports, creating a groove in the abutment body can increase the retention of the crown and reduce the amount of REC without weakening the abutment.6, 8 However, in this study, we found that the mean retention was higher in the group with 2 horizontal grooves as compared to other groups and lower in the ‘vertical groove’ group. Nonetheless, this failed to reach statistical significance when analyzed using the one-way ANOVA. This may be explained by the dimensions of the created grooves. Lewinstein et al. designed grooves during the construction of the abutment, which allowed them to design larger grooves.13 However, in this study, the abutments were prefabricated, and therefore it was not possible to create a deep groove without affecting the abutment body resistance. The use of cements of higher fracture strength in these conditions might reveal the effect of creating such grooves on increasing retention. In recent years, some studies reported the importance of creating grooves together with other modifications. In a recent study by Shrivastav, the influence of different surface modifications on the retention of a zinc phosphate cement-retained implant was investigated.20 The work investigated the effects of circumferential grooves with sandblasting (group 1) and with a bur modification (group 2) against control (group 3). It was shown that modifications in group 2 resulted in improving the retention of a bridge cemented on implant abutments.20 Sahu et al. reported that abutments with the milled and sandblasted modifications exhibited the highest retention, followed by abutments with retentive grooves, and then by abutments with the milled surfaces once the cast copings were cemented to implant abutments with a polymer-based cement.21
There are no specific guidelines available on the appropriate amount of cement to be used. Using a minimal amount of cement might decrease the cement rejection rate, but this method can result in problems such as inadequate retention and leakage.5, 9, 14 Similarly, excessive amounts of cement can cause problems such as the inappropriate placement of the coping and high REC values.14 However, the amount of cement used in this study was greater than the amount needed for flooding the relief space between the coping and the abutment. Although various methods have been proposed to adjust the appropriate cement amount, for clinicians, the control of the cement amount during the clinical stages is uncertain.22 Moreover, the amount of cement used in this study is the most commonly used for the cementation process by clinicians.10 Modified cementation methods are another option to reduce REC.11, 12 Such methods, despite being effective in reducing REC, might not be clinically feasible due to their time-consuming nature, especially in cases with higher number of implants. One method is to seat the restoration filled with cement on a mock abutment (an analog abutment) extraorally. This abutment could be a stock analog or a customized analog made from polyvinyl siloxane.14 Recently, Chee et al. explored 4 cementation methods for their effect on the amount of excess cement.12 They studied the cementation of the internal marginal area of the crown (group 1), cementation on the apical half of the axial walls of the crown (group 2), cementation to all axial walls of the interior surface of the crown, excluding the occlusal surface (group 3), and in group 4 – the crown filled with cement, and then seated on the putty index formed to the internal configuration of the restoration (a cementation device). The least amount of excess cement was found in group 4. The authors concluded that this method led to a uniform layer of the luting agent, which might be due to the internal surface of the crown leaving minimal excess cement when the restoration was seated.12
The creation of a vent hole in the restoration surface is also proposed to reduce REC.8, 13 Although this modification was introduced initially to reduce the seating discrepancies in tooth-supported restorations, it was found to have a negative effect on the integrity of the crown structure. Additionally, complex laboratory procedures are needed for its construction, after which it requires to be restored again by the dentist in the clinic.14 In a study by Wadhwani et al., a change in the abutment body as 2 opposite double-sided holes in the axial wall of the abutment was more effective than a normal abutment in decreasing REC, as the hole was used as a means to transfer cement to the abutment screw access space.6 In a finite element study by Rodriguez et al., an abutment design with 8 holes in the abutment margin area improved the pattern of the flow of cement into the abutment screw access space, thereby decreasing the rejection rate of the cement.8 Recently, Chen et al. tested the effect of a vent hole on the retentive force of a restoration. They showed that the retentive force of restorations with a vent hole was equal to or better than of those without a vent hole.23
Different methods have been proposed to block the abutment screw access hole, but there are currently no guidelines in this regard. Studies have shown that the partial filling of the screw access channel can act as a reservoir for excess cement and can also increase the retention of the restorations cemented with a temporary cement.24 In this study, some space within the abutment was preserved to prevent further rejection of cement and increase the retention, in addition to relative re-accessible blocking.
Unreliable retention is another concern about cemented restorations. The main factors affecting retention include abutment dimensions, framework properties and the characteristics of the cement used.14 In some circumstances, like small occlusogingival dimensions, where procedures are limited, other methods, such as changing the surface of the abutment body, are used.14
Changing the abutment surface texture by sandblasting also increases the retention of the crown, but this method is not quite feasible in commonly used implants. Additionally, the selective removal of the abutment walls increases retention by decreasing taper and creating vertical walls.10, 13, 14 However, this method increased the odds of abutment body weakening.
Conclusions
The purpose of the current study was to assess how different geometric changes in the dental implant abutment body influence the amount of REC and the retention of cemented implant-supported prostheses. It was found that the REC means in groups 2 (1 horizontal groove) and 3 (2 horizontal grooves) were statistically significantly different from control group 4 (no grooves) (p < 0.05). There was a significant difference between the lowest mean REC value (group 1) and the highest mean REC value (group 3) (p < 0.05). However, 1 and 2 horizontal grooves in the abutment body effectively reduced REC in comparison with other groups.