Abstract
Background. The impact of dynamic fatigue loading on denture adaptation and retention is clinically important. Zirconia and cobalt–chromium (Co–Cr) frameworks enhance denture strength, but their performance under cyclic loading remains unclear.
Objectives. The aim of the study was to evaluate the adaptation and retention of maxillary single dentures reinforced with digitally constructed Co–Cr or zirconia frameworks after a simulated 1 year of function.
Material and methods. Three types of maxillary single dentures were constructed on maxillary master casts. Group A included maxillary dentures without reinforcement (control group), whereas groups B and C encompassed maxillary dentures reinforced with digitally designed and milled Co–Cr and zirconia frameworks, respectively (n = 13/group). Acrylic resin was conventionally processed on stone casts. Initial adaptation was evaluated for each denture using Geomagic software, which allowed for accurate matching and superimposition of the scanned master cast with the standard tessellation language (STL) file of the scanned fitting denture surface obtained with the use of a desktop scanner. Initial retention was evaluated using a universal testing machine. Dynamic fatigue loading of 50 N at a speed of 60 mm/s was applied in the chewing simulator, after which final adaptation and retention values were recorded. Paired t-tests were conducted to compare results within each group, and one-way analysis of variance (ANOVA) was performed to compare the 3 groups. When ANOVA revealed significant differences, Tukey’s honestly significant difference (HSD) test was used for post hoc pairwise comparisons. The significance level was set at p ≤ 0.05.
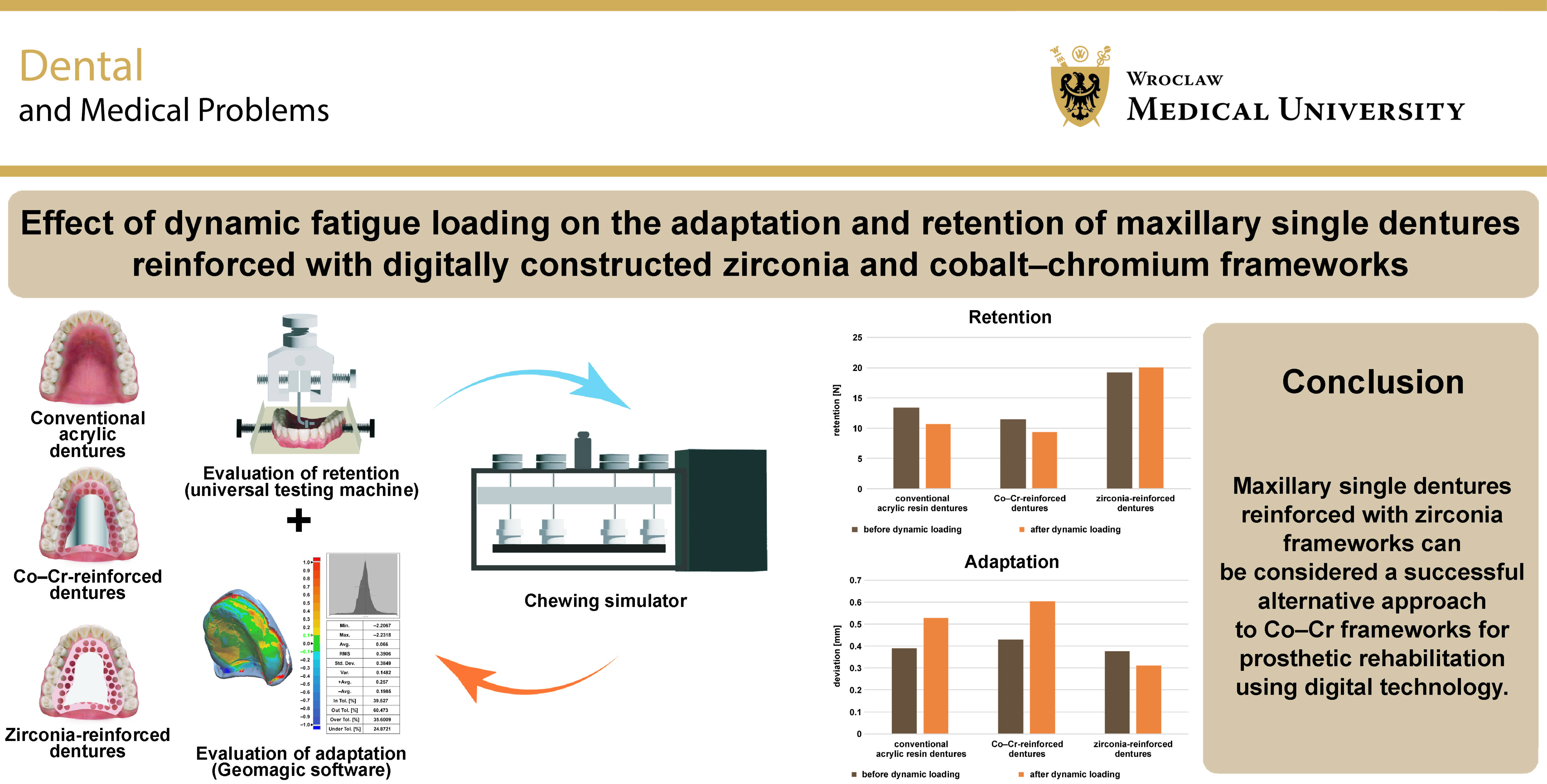
Results. Group C showed the most favorable adaptation after dynamic fatigue loading (0.31 ±0.04 mm), while group B exhibited the least favorable adaptation (0.61 ±0.08 mm). Regarding retention, group C demonstrated the highest values (20.04 ±0.96 N), while group B exhibited the lowest values (9.32 ±0.78 N). Significant differences were observed among the 3 groups for both adaptation and retention.
Conclusions. Maxillary single dentures reinforced with zirconia frameworks may represent a successful alternative to Co–Cr frameworks for prosthetic rehabilitation using digital technology.
Keywords: zirconia, retention, adaptation, Co–Cr, reinforced maxillary single denture
Introduction
Maxillary single dentures opposing mandibular natural teeth pose challenges in achieving adequate comfort, retention, function, and esthetics.1 The most common complication associated with maxillary dentures is fracture, especially in the presence of natural mandibular teeth. The predominant mode of failure is flexural fatigue caused by cyclic deformation due to masticatory forces, typically resulting in a midline fracture of the denture.2, 3
The most commonly used material for the fabrication of dentures is acrylic resin, specifically polymethyl methacrylate (PMMA). Polymethyl methacrylate has gained widespread acceptance among patients due to its favorable mechanical, biological and esthetic qualities. Compared with metal denture bases, PMMA denture bases are easier to construct and repair.1 However, PMMA dentures are susceptible to failure due to their low fatigue resistance. Midline fractures are a frequent complication, often resulting from occlusal disharmony, flexure and fatigue of the denture base.1 Reinforcing materials can be used to enhance the mechanical properties of maxillary dentures. Therefore, the implementation of reinforced denture bases has been proposed as a potential solution.4, 5, 6, 7
Cobalt–chromium (Co–Cr) alloys are primarily used as metal reinforcement materials to improve the stability and fracture resistance of single dentures. These alloys show excellent mechanical properties, biocompatibility and corrosion resistance.8 However, their rough surface and susceptibility to internal defects, as well as difficult casting procedures may lead to unexpected complications.8, 9
Advances in digital technology and the development of computer-aided design and computer-aided manufacturing (CAD/CAM) have enabled the production of Co–Cr prostheses through computer numerical control milling, eliminating casting-induced porosity and manufacturing defects.10
Recent trends in prosthetic dentistry favor metal-free restorations. Metal frameworks are heavier and require more complicated fabrication procedures, as well as pose a risk of hypersensitivity due to their alloy composition.11
A newer generation of zirconia, ceria-stabilized zirconia/alumina (Ce-TZP/Al2O3), is a nanocomposite in which nanometer-sized alumina particles and ceria-stabilized zirconia particles are dispersed within ceria-stabilized zirconia crystal and alumina crystal, respectively.12, 13 Ceria-stabilized zirconia/alumina demonstrates excellent mechanical properties, including high flexural strength, high fracture toughness and high resistance to low-temperature degradation.14, 15, 16, 17 These characteristics exceed those of conventional yttria-stabilized zirconia (Y-TZP), and its elastic modulus is comparable to that of Co–Cr alloys, suggesting potential applicability of Ce-TZP/Al2O3 as a denture base material and a possible substitute for metal alloys.13
The present study was conducted to assess whether reinforcement of a maxillary single denture with digitally constructed Co–Cr or zirconia frameworks affects denture retention and adaptation. Additionally, the effect of these frameworks after dynamic fatigue loading simulating 1 year of function was assessed using a chewing simulator. The null hypothesis posited that there are no variations between conventional and reinforced maxillary single dentures in terms of adaptation and retention.
Material and methods
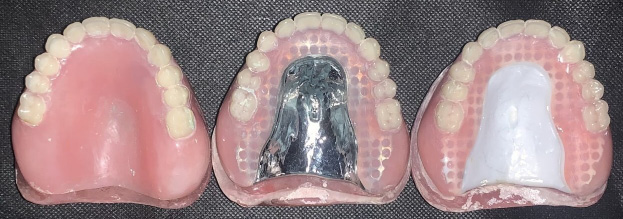
Three types of maxillary single dentures were constructed on maxillary master casts obtained from patients requiring maxillary single dentures. The maxillary arch presented a U-shaped residual alveolar ridge without bony or soft tissue undercuts. Group A included conventional acrylic resin maxillary single dentures without reinforcement (control group), group B encompassed maxillary single dentures reinforced with a digitally designed and milled Co–Cr framework, and group C comprised maxillary single dentures reinforced with a digitally designed and milled zirconia framework (Figure 1).
The study was reviewed and approved by the Research Ethics Committee of the Faculty of Dentistry, Ain Shams University, Cairo, Egypt (approval No. FDASU-RecID041914).
Master cast preparation and maxillary single denture fabrication
Thirteen definitive master casts were obtained from the patients. The geometric center of each arch was determined. The midline of the cast was drawn from the center of the incisive papilla to a point located in the middle of a line connecting the 2 hamular notches. Then, a midpoint was marked on the midline to represent the center of the arch.18, 19 The definitive master casts were fixed on a plate inside a desktop scanner with their labial surfaces facing the interior of the scanner (D850; 3Shape, Copenhagen, Denmark). The scanning procedure followed the software protocol. Subsequently, the casts were duplicated using a silicone base duplication material (REPLISIL 22 N; dent-e-con, Lonsee, Germany) to obtain 39 duplicate stone master casts (n = 13/group), on which the 3 types of maxillary single dentures were constructed.
Acrylic unreinforced maxillary single dentures (group A) were constructed using the conventional method on the duplicate stone master casts and served as reference dentures to standardize the acrylic thickness and tooth positioning during the fabrication of dentures reinforced with Co–Cr and zirconia frameworks (groups B and C).20 A rubber index of the maxillary teeth and the polished surface of the flanges was prepared for each acrylic denture.
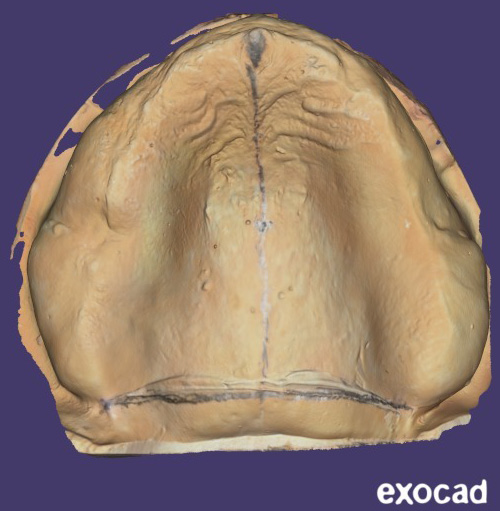
The object replacement character (OBJ) files of the scanned definitive master casts were imported into the digital design software partial module (PartialCAD; exocad GmbH, Darmstadt, Germany) to design the reinforcement frameworks for groups B and C (Figure 2). The frameworks were virtually relieved with a 0.5-mm thickness wax on the crest of the ridge with tissue stops and on the median palatine raphe. It was designed to cover the palatal area with an extended palatal plate, a major connector and a mesh denture base extending to the crest of the ridge. The framework thickness was set at 1.5 mm.20 An attachment was placed at the geometric center of the polished surface of the framework, corresponding to the previously marked point on the cast (Figure 3).
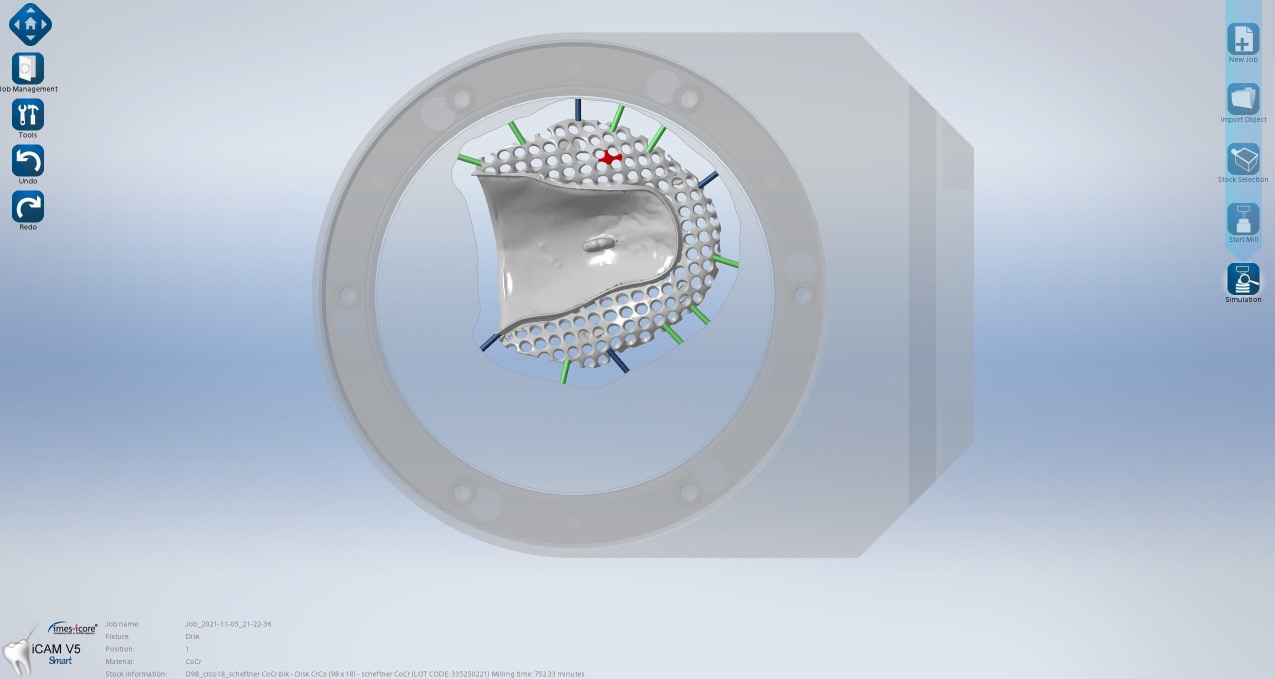
The standard tessellation language (STL) files of the design were imported into the CAM software (iCAM V5 smart; imes-icore GmbH, Eiterfeld, Germany) and milled in both Co–Cr and zirconia frameworks using a 5-axis dry and wet milling machine (CORiTEC 350i; imes-icore GmbH).
For Co–Cr framework milling (group B), the design was nested in a 98 mm × 18 mm pre-sintered Co–Cr blank (MoguCera C Disc; Scheftner, Mainz, Germany) (Figure 4). Dry milling of the Co–Cr disk was performed using burs of different sizes. The average milling time was 752.33 min Polishing was performed with the use of a polishing lathe and cloth brushes.
For zirconia framework milling (group C), the design was nested in a 98 mm × 25 mm zirconia blank (Nacera®; DOCERAM Medical Ceramics GmbH, Dortmund, Germany) with a scale factor of 1.25 (Figure 5). The zirconia disks were dry milled, with an average milling time of 300.23 min. Subsequently, complete sintering was performed in a furnace at 1,350–1,500°C to achieve their final shape.
With the aid of the rubber index, 2 reinforced maxillary dentures, with the same tooth position as conventional unreinforced dentures, were constructed on duplicate stone master casts. Zirconia and Co–Cr frameworks were fixed to the duplicated master casts using a quick-drying glue to prevent deformation. Teeth were set within the index, and the acrylic resin was carefully packed and processed in a conventional manner.21
Construction of resin casts with mucosa simulation
The definitive maxillary master casts were modified to construct resin casts with simulated mucosa, which served as models for the evaluation of retention and dynamic fatigue loading. A vacuum sheet was processed on the cast to fabricate a stent with 3 tissue stops. The cast surface was then reduced by 2 mm to create space for the tissue-simulating mask. The modified cast was duplicated to obtain 3 polyurethane epoxy resin casts (Exakto-Form; bredent medical GmbH & Co. KG, Senden, Germany) using a silicone mold. An adhesive was applied to the epoxy casts, and a silicone mucosa gingival mask with viscoelastic properties similar to those of palatal mucosa (Multisil; bredent medical GmbH & Co. KG)22 was injected into the stent and pressed onto the epoxy cast to simulate the mucosa. Therefore, for each denture, an epoxy resin master cast with soft tissue simulation was constructed.
Evaluation of initial adaptation
All dentures were lightly coated with antiglare spray before scanning their fitting surfaces using the desktop scanner (D850; 3Shape) to obtain STL files. The STL files were imported into the Meshmixer software (https://meshmixer.org) to invert the fitting surfaces so that they resembled cast surfaces.23
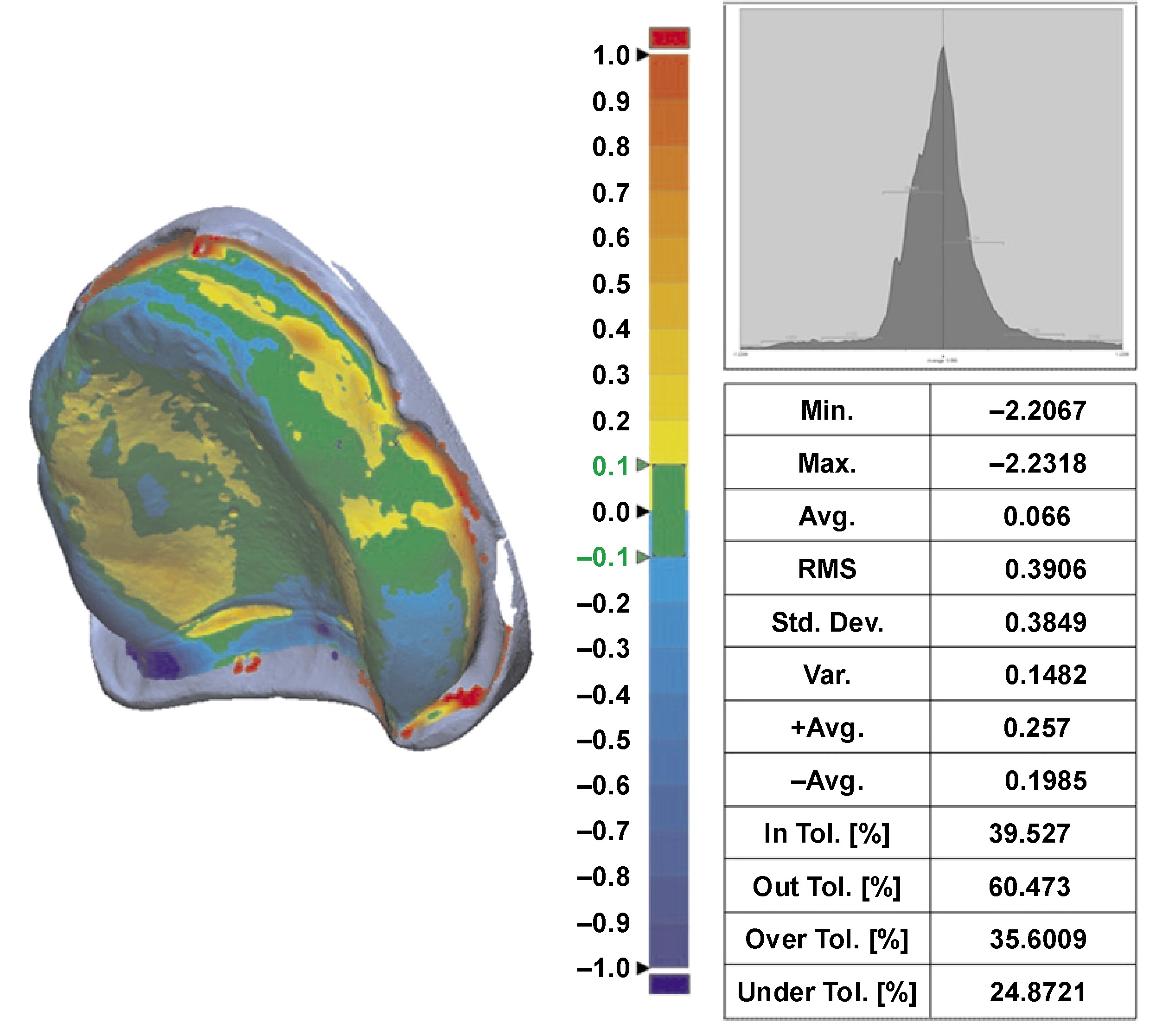
The Geomagic software (Geomagic Control X64; Hexagon Manufacturing Intelligence, LLC, Morrisville, USA) was used to evaluate the adaptation of the maxillary denture bases to the scanned master cast. The STL files of the master cast and the inverted fitting surface were imported into the software. Then, the STL file of the denture fitting surface was superimposed onto the STL file of the orresponding master cast.23 Alignment between the reference and measured data was performed automatically using the best-fit alignment option. The 3D Compare function was used to evaluate the adaptation of the measured data. The results were presented as both a color scale and numerical values (Figure 6). Adaptation was interpreted based on the distance between the fitting surface of the denture base and the reference data.
Evaluation of initial retention
A metallic ring was attached to the geometric center of the polished surface of the denture bases using self-curing acrylic resin. Artificial saliva was prepared according to the Glandosane formula by the Laboratory of the Pharmaceutical Industry at the Faculty of Pharmacy, Ain Shams University, Cairo, Egypt, and placed between the cast and the denture. A pressure of 98 N was applied to the dentures for 20 s to spread the artificial saliva uniformly across the entire mucosal surface of the denture base. The epoxy resin cast with mucosa simulation was secured to the lower component of a universal testing machine (Instron 3365; Instron®, Norwood, USA) with the palate facing upward. Tensile force was applied to the attached ring in an upward direction perpendicular to the imaginary occlusal plane (Figure 7). The crosshead speed of the universal testing machine was set at 50 mm/min. Retention was defined as the maximum traction force required to separate the denture base from the maxillary cast. The test was conducted 10 times, and the mean value of the 10 measurements was recorded as the retention force.
Dynamic fatigue loading
Each denture was seated on its corresponding epoxy resin cast and placed in a chewing simulator (CS-4; SD Mechatronik, Feldkirchen-Westerham, Germany) (Figure 8). Dynamic cyclic loading was applied by means of a stylus falling at the center of the metal plate that was previously attached to the occlusal surface of the denture at the center of the arch. The applied load was set at 50 N, and the software parameters were as follows: a speed of 60 mm/s; a vertical path of 3 mm; a horizontal path of 0.7 mm; and a frequency of 1.6 Hz. Each denture was subjected to biaxial cyclic loading for a total of 250,000 cycles, which represented 1 year of intraoral function.21
After the chewing simulation, all procedures for measuring adaptation and retention were repeated for the 3 groups as previously described.
Statistical analysis
The sample size was calculated using the G*Power software for Windows (v. 3.1.9.4; https://www.psychologie.hhu.de/arbeitsgruppen/allgemeine-psychologie-und-arbeitspsychologie/gpower). A sample size of 12 dentures per group was determined to detect significant differences with a statistical power of 95% (α = 0.05). The sample size was subsequently increased to 13 dentures per group to compensate for potential dropouts.
The obtained data was recorded, tabulated and statistically analyzed. Paired t-tests were applied to compare results within each group, and one-way analysis of variance (ANOVA) was performed to compare the 3 groups. Tukey’s honestly significant difference (HSD) test was used for post hoc pairwise comparisons when the results of ANOVA indicated significant differences. The significance level was set at p ≤ 0.05. Statistical analyses were performed using the IBM SPSS Statistics for Windows software, v. 20.0 (IBM Corp., Armonk, USA).
Results
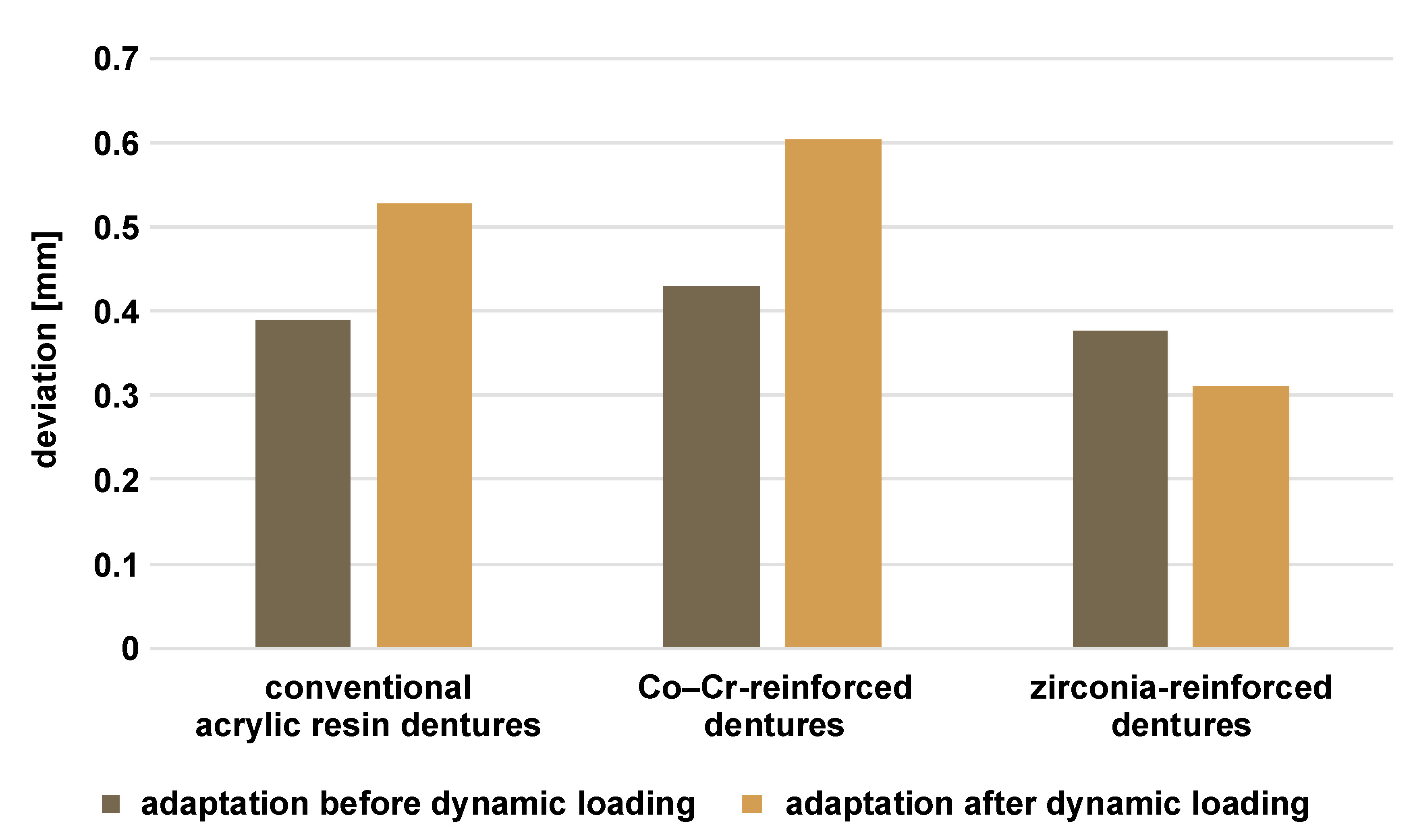
Regarding the effect of dynamic fatigue loading on the adaptation within each group, the deviation from the scanned master cast increased in group A (conventional acrylic resin) and group B (Co–Cr framework), indicating reduced adaptation. In contrast, group C (zirconia framework) showed less deviation from the scanned master cast, indicating better adaptation. These changes were statistically significant according to the results of the paired t-test (Table 1, Figure 9).
When adaptation was compared between the 3 groups before dynamic fatigue loading, only minimal differences were observed, with group C demonstrating slightly more favorable adaptation. However, these differences were not statistically significant according to ANOVA. After dynamic fatigue loading, group C exhibited the best adaptation, while group B demonstrated the least favorable adaptation. These changes were statistically significant based on the outcomes of ANOVA. Tukey’s post hoc HSD test revealed significant differences between groups A and B, groups A and C, and groups B and C (Table 1, Figure 9).
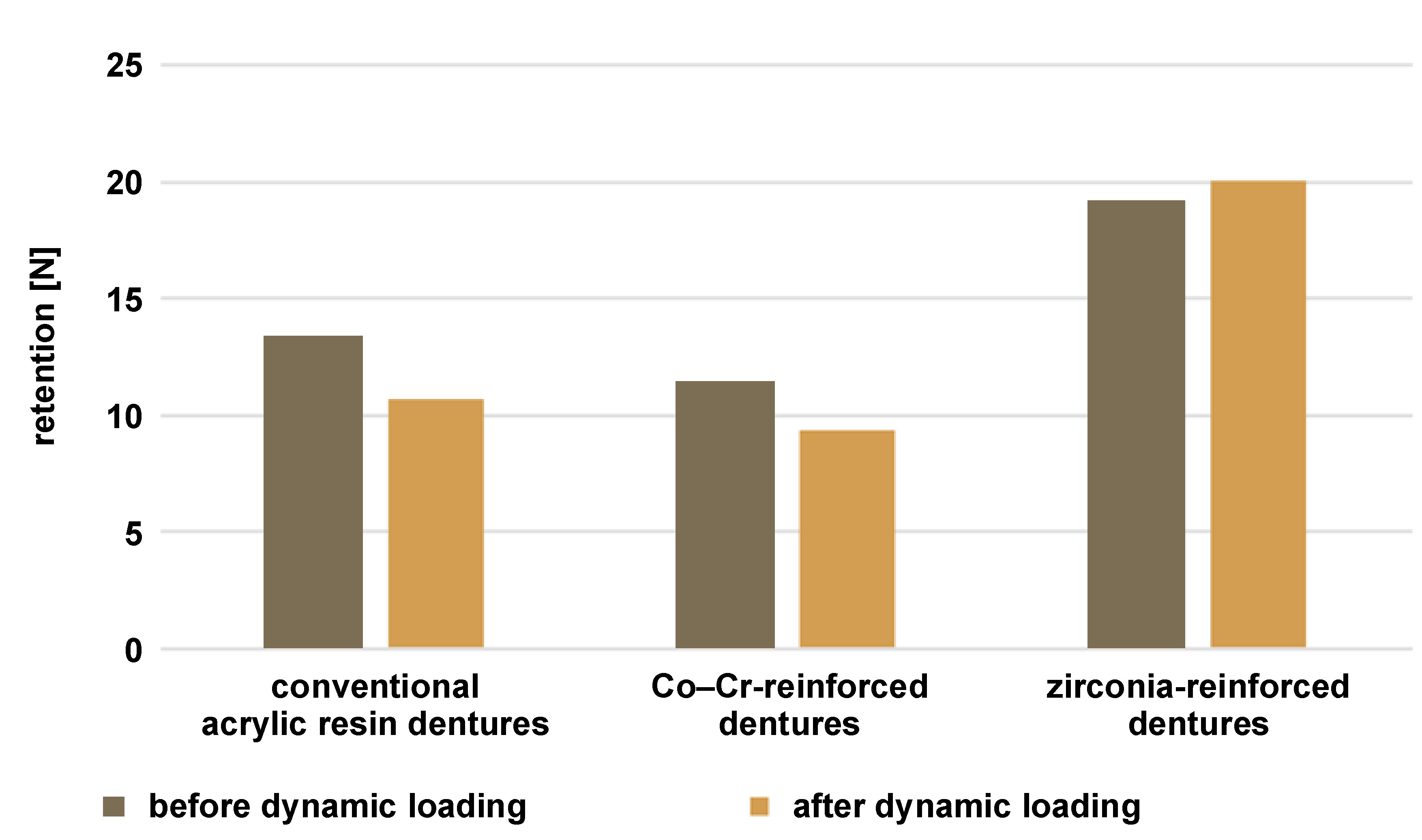
Regarding the effect of dynamic fatigue loading on retention within each group, retention decreased in groups A and B after loading, whereas it increased in group C. These changes were statistically significant based on the results of the paired t-test (Table 2, Figure 10).
Comparison of retention among the 3 groups before and after dynamic fatigue loading revealed that group C achieved the highest retention values, while group B exhibited the lowest retention. These differences were statistically significant according to ANOVA. Tukey’s post hoc HSD test indicated significant differences between groups A and B, groups A and C, and groups B and C (Table 2, Figure 10).
Discussion
The present study aimed to evaluate the retention and adaptation of reinforced maxillary dentures fabricated using CAD/CAM with Co–Cr and zirconia frameworks, compared with conventional acrylic resin dentures, before and after dynamic fatigue loading. Adequate denture adaptation contributes to good retention, stability and support.24
Definitive master casts were obtained from patients to include a diverse range of residual alveolar ridge shapes and forms. These anatomical variations were carefully considered during the design and execution of the crossover study. However, it is crucial to emphasize that these variations did not introduce bias or significantly influence the study outcomes. A similar approach was reported by Faty et al. and Abd El Galil et al., 23, 25 who incorporated casts from different patients to evaluate denture adaptation and retention.
The geometric center of the arch was manually determined on the definitive master cast before scanning and later transferred to the framework design for standardization. While digital application during the design process of both frameworks would provide greater accuracy, transferring this position to the conventional denture was difficult.23 The geometric center was chosen to measure the retention of the denture base based on previous studies reporting this region as the most reliable for testing the retention of maxillary complete dentures.26, 27
A desktop scanner (D850; 3Shape) with a camera resolution of 5 MP and an accuracy of 4 μm was used. This open system allows data export to the PartialCAD software.25 The definitive master cast scans were exported to OBJ files and imported into the PartialCAD module to preserve the drawn data on the cast. A plate design was used to reinforce the maxillary denture rather than a mesh or wire embedded within the acrylic denture base. It was found that the use of metal wire reinforcement inhibits polymerization and thermal shrinkage of the dough resin during denture construction, thereby compromising denture adaptation.28
A 5-axis dental milling machine (CORiTEC 350i; imes-icore GmbH) was used to construct the frameworks. This system offers advantages over conventional 3-axis machines. It enables movement in 3 spatial directions, in addition to rotational movement along the 4th axis. Additionally, the milling spindle of this machine can rotate, providing the 5th axis of motion. These combined functionalities facilitate the milling process of complex geometries with subsections.29 Different bur sizes were used, as large burs provide good durability and an excellent cutting rate, while smaller burs allow accurate reproduction of fine details. Precise cutting is an important factor in the CAD/CAM milling process.30
Denture adaptation was evaluated using the Geomagic software, a surface-matching program that enables superimposition of 2 surfaces to determine deviations between them.24 The calculated mean values might be close to 0, which is non-practical, indicating a perfect fit. Therefore, the root mean square (RMS) values were used to eliminate the influence of positive and negative signs.31, 32
A gingival mask with viscoelastic properties similar to those of oral mucosa and minimal dimensional change or permanent deformation was used during retention measurements and chewing simulation. To ensure a stable non-movable model surface, the gingival mask was bonded to the underlying model using an adhesive.33 During chewing simulation, the load was applied to the center of a metal plate. Metal was selected instead of acrylic due to its superior stress distribution properties, as demonstrated in previous studies.34, 35, 36 The simulation consisted of 2,500,000 chewing cycles, representing approx. 1 year of dental function.37 During the retention measurements and chewing simulation, Glandosane artificial saliva was employed. Artificial saliva simulates oral conditions and influences the biological properties of the materials, while also removing debris resulting from material wear.38, 39 Bayer et al. demonstrated that the absence of saliva can alter frictional wear, consequently affecting retention force values.40
Hwang et al. reported an acceptable range for adaptation deviation, ranging between 0.05 mm and 0.30 mm.41 In the present study, before dynamic fatigue loading, all maxillary single dentures demonstrated acceptable adaptation values, with no statistically significant differences observed between the groups. Hence, all methods may be considered suitable for restoring single maxillary arches. However, subjecting the dentures to dynamic fatigue loading revealed a statistically significant difference among the groups, leading to the rejection of the null hypothesis. Among the tested groups, group C (zirconia framework) exhibited the best adaptation, which may be attributed to the high flexural and bending strength of nanozirconia (900–1,200 MPa).42 These values surpass those of milled Co–Cr (480 ±20 MPa)43 and conventional acrylic resin (624.6–825.4 MPa).44 On the other hand, the adaptation of group A (conventional acrylic resin) decreased after dynamic fatigue loading, Notably, our study demonstrated that group A showed better adaptation than group B (Co–Cr framework). This difference may be attributed to water absorption of acrylic resin during the experimental period.45, 46
In a study conducted by Amaral et al., the flexural strength of surface-treated Y-TZP disks was evaluated before and after mechanical cycling.47 The researchers observed a phase transformation from the tetragonal to monoclinic phase, resulting in the creation of a superficial compression layer that enhanced surface toughness and increased initial flexural strength. Regarding Co–Cr alloys, hard milling of Co–Cr blocks minimized the occurrence of casting defects.48 However, Kim et al. concluded that milled Co–Cr exhibited inferior mechanical properties and was considered the least favorable method for Co–Cr manufacturing.43 This was attributed to the presence of a large grain size in milled Co–Cr, which adversely affected its mechanical properties, particularly yield strength.
In the present study, all groups demonstrated acceptable retention values. However, zirconia-reinforced dentures (group C) exhibited the highest retention both before and after dynamic fatigue loading. This finding can be explained by the well-established relationship between complete denture retention and good denture base adaptation, as reported in numerous studies.4, 49, 50 Thus, the observed retention results are consistent with the findings related to adaptation.
Limitations
Several limitations of the present study should be acknowledged. Laboratory methods and results may not fully reflect clinical performance. Although the chewing simulator provided a controlled environment for evaluating denture adaptation and retention, it could not fully replicate the complex and dynamic oral conditions experienced by patients in real-life situations. Factors such as variations in salivary flow, oral muscle activity and oral hygiene practices may influence denture behavior in the clinical setting. Therefore, caution should be exercised when extrapolating these findings to clinical practice. Further research, including clinical studies with long-term follow-up, is required validate the results of this laboratory-based investigation.
Conclusions
Maxillary single dentures reinforced with zirconia frameworks can be considered a successful alternative approach to Co–Cr frameworks for prosthetic rehabilitation using digital technology.
Ethics approval and consent to participate
The study was reviewed and approved by the Research Ethics Committee of the Faculty of Dentistry, Ain Shams University, Cairo, Egypt (approval No. FDASU-RecID041914).
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.
Use of AI and AI-assisted technologies
Not applicable.